Unit 1: Foundations of Longevity Coaching¶
Chapter 1.4: Assessment & Biomarkers¶
[CHONK: 1-minute summary]
What you'll learn in this chapter:
- Which tests matter for longevity tracking (and which are optional)
- How to interpret results within coaching scope: what you can say, what needs referral
- How to conduct Deep Health assessments across all six dimensions
- How to use assessment data to motivate clients and guide coaching conversations
The big idea: You can't coach longevity without measuring it. But assessment isn't just about collecting numbers. It's about knowing what those numbers mean (and what they don't mean), staying within your scope, and using data to personalize your approach. This chapter teaches you the essential biomarkers, functional tests, and subjective assessments that form the foundation of evidence-based longevity coaching.

Figure: Biomarkers + Functional + Subjective
Introduction¶
Assessment is the foundation of effective longevity coaching because it replaces guessing with clarity. When you measure, you can see where clients are starting, whether interventions are working, and what to prioritize next.
What new coaches often miss is that assessment isn't just about tests and numbers. It's about understanding what those numbers mean, and equally important, what they don't mean, so you can talk about results confidently while knowing when it's time to loop in a doctor.
This chapter covers:
1. Functional metrics: the tests you can help clients improve (VO2 max, grip strength, movement tests)
2. Imaging and blood panels: what they measure and how to discuss results in scope
3. Deep Health assessments: the subjective side that objective tests miss
4. Putting it together: creating practical assessment protocols for real clients
One principle guides everything: screen, don't diagnose. You can recommend tests, discuss trends, and explain what numbers generally mean, but you cannot diagnose conditions or prescribe treatments. That line keeps you in scope and protects your clients.
[CHONK: Functional Metrics - The Tests You Can Actually Improve]
Functional Metrics — The Coach's Power Zone¶
Functional metrics are special: they predict longevity AND you can directly help clients improve them, which means they're not just assessment tools but intervention targets.
VO2 Max: The Strongest Mortality Predictor¶
VO2 max measures your body's maximum ability to use oxygen during exercise. It's the single strongest predictor of all-cause mortality among all biomarkers.¹
The numbers are striking: people with the highest cardiorespiratory fitness have approximately 53% lower all-cause mortality compared to those with the lowest fitness.² Each 1-MET increase associates with 11-17% lower mortality risk.³
Target: The Longevity Protocol recommends 35+ mL/kg/min as a longevity goal. This is achievable for most people with consistent aerobic training.
How to measure:
- Lab testing: Direct measurement with respiratory gas analysis (gold standard, expensive)
- Field tests: Cooper 12-minute run, step tests (accessible, valid for tracking trends)
What coaches can say: "Higher VO2 max is associated with longer life. The research is clear: fit people live longer. We can improve yours through consistent aerobic training: Zone 2 work most days, plus some higher-intensity intervals."
Refer when: Client experiences chest pain, dizziness, or abnormal symptoms during testing.
Grip Strength: A Window into Overall Health¶
Grip strength isn't just about your hands; it's a proxy for overall muscle function throughout the body.
Lower grip strength consistently predicts higher mortality. People in the highest tertile have 59-62% lower mortality risk compared to the lowest tertile.⁴ Each 1-kg increase in grip strength associates with 2-10% reduced mortality risk depending on population.⁵
Thresholds: The EWGSOP2 guidelines define probable sarcopenia at <27 kg for men and <16 kg for women.
Tracking target: Weekly grip testing with a goal of 70+ pounds as a strength proxy.
What coaches can say: "Grip strength reflects your overall muscle function. Research shows weaker grip predicts higher mortality. If your grip is low, that tells us to focus on whole-body strength training, not just your hands."
Refer when: Grip dramatically below thresholds, especially with other signs of muscle loss (difficulty rising from chairs, unexplained weight loss).
Movement Tests: Simple, Free, Highly Predictive¶
These tests require no equipment and predict mortality surprisingly well.
Sit-to-rise test: Start seated on the floor, rise to standing without using hands or knees. Each support point used subtracts from score.
- Lower scores predict higher mortality. The lowest scores showed 5.44 times higher mortality risk over 6.3 years⁶
- Each 1-point improvement associates with ~21% better survival
Timed Up-and-Go (TUG): Rise from chair, walk 3 meters, turn, walk back, sit down.
- ≥9 seconds indicates higher risk, approximately 2.66 times higher mortality⁷
- Each additional second associates with ~5% increased mortality
Gait speed: Simple walking speed.
- Each 0.1 m/s slower associates with 12% higher mortality⁸
| For DIY Learners |
|---|
| Applying this to yourself: Try the sit-to-rise test right now. Sit on the floor, then stand up using as little support as possible. Score 5 points for sitting and 5 for rising, subtracting 1 point each time you use a hand, knee, forearm, or side of leg for support. A score below 8 suggests you'd benefit from focused mobility and strength work. This isn't about judgment: it's about knowing where you are so you can improve. |
One-legged stance: Balance on one leg for 10 seconds.
- Inability to complete predicts 1.84 times higher mortality over 7 years⁹
What coaches can say: "These tests show how well your body moves and functions. People who score well live longer. The good news: strength training, balance work, and mobility exercises all improve these scores."
Refer when: Client can't safely attempt tests (high fall risk, severe balance issues).
[CHONK: Coaching in Practice - Assessment Resistance]
Coaching in Practice: "I Don't Want to Know My Numbers"¶
The scenario: Patricia, 54, wants to "feel better," but she resists any testing. "I already know I'm out of shape, so why do I need a test to tell me that?"
What NOT to do:
❌ "Testing is essential for longevity coaching. We really need baseline data."
Why it doesn't work: You’ve made it about your needs, not hers, so she’ll likely dig in deeper.
What TO do:
✅ Acknowledge the resistance, then reframe assessment as empowerment.
Sample dialogue:
Coach: "I hear you, and it sounds like you’re worried about seeing numbers you won’t like, right? That’s totally reasonable."
Patricia: "Yeah, exactly. I’ll just feel worse about myself."
Coach: "That makes sense. Here's what I've noticed: when people avoid testing, they're usually guessing, and often guessing wrong. You might feel "out of shape," but we don't actually know yet which parts of your health need attention most."
Patricia: "I mean... I know my cardio is bad."
Coach: "Maybe, and it's also possible your cardio is better than you think, while strength is what we should focus on first, or even balance. Testing isn't about making you feel bad; it's about showing us where to focus so your effort pays off. What if we started with something simple like grip strength, which takes about 30 seconds, and we treat it as information, not a grade? Would you be willing to try just that one thing?"
Patricia: "I guess grip strength doesn't sound too scary."
Coach: "Perfect. We'll start there, build some trust, and then decide together if we want to add more later."
Key takeaway: Start with the least threatening test and build trust before moving into a full assessment.
[CHONK: Imaging and Blood Panels]
[CHONK: Imaging and Blood Panels]
Imaging Tests¶
DEXA Scans: Body Composition and Bone Health¶
DEXA measures three things that matter for longevity:
- Bone mineral density (BMD): an indicator of fracture risk.
- Body composition: lean mass, fat mass, and body fat percentage.
- Visceral adipose tissue (VAT): the fat around organs that’s linked with higher health risk.
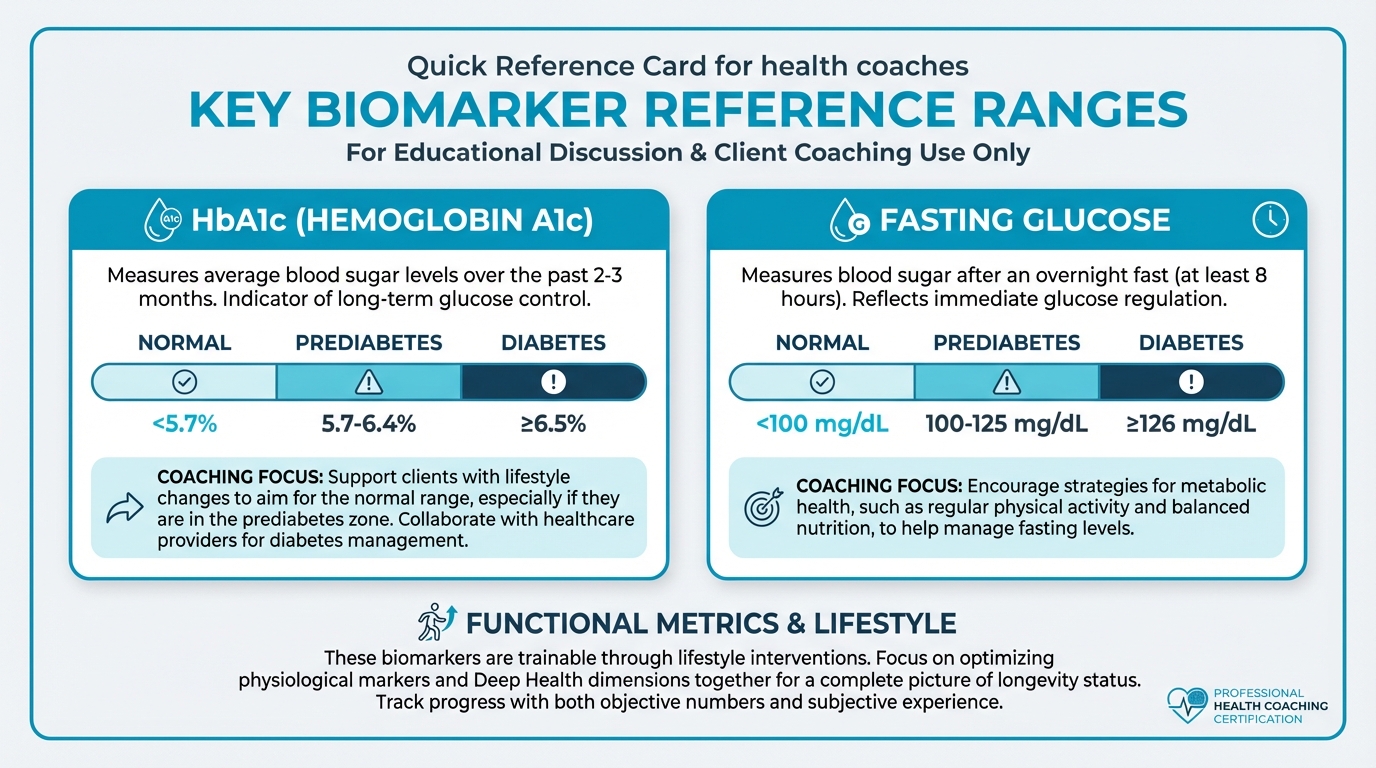
Figure: Normal/optimal ranges for key markers
Body composition coaching (what not to do):
- Client: “So… is this good or bad?”
- Coach: “Your DEXA says your visceral fat is bad. You need to lose it.”
Body composition coaching (better, as a dialogue):
- Client: “So… what does this scan actually tell me?”
- Coach: "Great question. Your DEXA shows how much muscle and fat you have, and where the fat is stored. In general, higher muscle mass and lower visceral fat tend to be associated with better longevity outcomes. We'll use today's numbers as a baseline and track how they change as we work on your habits."
Bone density coaching (what not to do):
- Client: “What does my T-score mean?”
- Coach: “Your T-score means you have osteoporosis.”
Bone density coaching (better, as a dialogue):
- Client: “Does this mean something is wrong with my bones?”
- Coach: "Your DEXA includes bone density measurements, but your doctor should interpret the T-score for any medical diagnosis. What I can do is support the lifestyle side: strength training, plus adequate protein and calcium, all support bone health."
T-scores (for reference, not diagnosis):
- Normal: ≥ -1.0
- Osteopenia: -1.0 to -2.5
- Osteoporosis: ≤ -2.5
Refer when: T-score ≤ -2.5, rapid bone density decline, or any questions about medical implications.
Frequency: Annually for body composition; every 2-3 years for bone density.
Blood Panels¶
Blood panels give you a window into metabolic health, inflammation, and cardiovascular risk. One key reminder: you cannot independently interpret medical lab results. You can talk about trends, lifestyle connections, and general education, but medical interpretation belongs to physicians.
Metabolic Markers¶
HbA1c: the average blood sugar over 2-3 months.
- Normal: <5.7%
- Prediabetes: 5.7-6.4%
- Diabetes: ≥6.5%
Fasting glucose: blood sugar after an overnight fast.
- Normal: <100 mg/dL
- Prediabetes: 100-125 mg/dL
- Diabetes: ≥126 mg/dL
Metabolic markers coaching (what not to do):
- Client: “So does this mean I’m insulin resistant?”
- Coach: “Your numbers are high, so you’re insulin resistant. Cut carbs immediately.”
Metabolic markers coaching (better, as a dialogue):
- Client: “Are these numbers bad?”
- Coach: "These markers reflect blood sugar control, and higher values can suggest insulin resistance, meaning your body isn't responding to insulin efficiently. Your physician is the right person to diagnose anything medical, and I can help you work on the parts we can control day to day: nutrition and exercise, which improve insulin sensitivity."
Refer when: HbA1c ≥6.5% or fasting glucose ≥126 mg/dL (diabetes range).
Inflammatory Markers¶
hsCRP: high-sensitivity C-reactive protein, which measures chronic inflammation.
- Low risk: <1 mg/L
- Average risk: 1-3 mg/L
- High risk: >3 mg/L
Inflammation coaching (what not to do):
- Client: “My hsCRP is high. What does that mean?”
- Coach: “Your inflammation is high, so you’re aging faster.”
Inflammation coaching (better, as a dialogue):
- Client: “Should I be worried about this hsCRP?”
- Coach: "Higher inflammation is associated with accelerated aging, but it's also one of the areas where lifestyle can make a real difference. Lifestyle changes—exercise, anti-inflammatory nutrition, stress management, quality sleep—can help reduce chronic inflammation."
Refer when: Very high values (>10 mg/L) may indicate acute infection or autoimmune conditions.
Lipids¶
ApoB: the number of atherogenic particles (often considered a particularly helpful marker for cardiovascular risk).
Traditional panel: total cholesterol, LDL, HDL, triglycerides.
Lipids coaching (what not to do):
- Client: “Do I need medication?”
- Coach: “Your cholesterol is off. You need meds.”
Lipids coaching (better, as a dialogue):
- Client: “What do these lipid numbers mean for me?”
- Coach: “These markers relate to cardiovascular risk. Your physician will guide any medication decisions, and we can focus on the lifestyle side. Lifestyle changes—regular exercise, Mediterranean-style eating, maintaining healthy weight—can positively impact these numbers. We’ll also watch trends over time, not just a single lab draw.”
Refer when: Very elevated values, need for medication decisions, concerning trends despite lifestyle changes.
Hormones: Medical Territory¶
Hormone panels (testosterone, estrogen, thyroid) require physician interpretation. Coaches should not interpret hormone results or recommend hormone optimization.
Hormones coaching (what not to do):
- Client: “My testosterone is low. What should I do?”
- Coach: “Your testosterone is low. Let’s optimize your hormones.”
Hormones coaching (better, as a dialogue):
- Client: “I’m tired all the time. Should I get my hormones checked?”
- Coach: "Hormone levels do change with age, and symptoms like fatigue, mood changes, or low energy are worth discussing with your doctor. I can't interpret hormone labs, but I can support your overall health through lifestyle like exercise, sleep, and stress management, which all influence hormone function."
[CHONK: Coaching in Practice - Blood Work Discussion]
Coaching in Practice: Discussing Blood Results¶
The scenario: Marcus, 51, brings his lab results: HbA1c is 6.2% (prediabetic), hsCRP is 3.8 (elevated), and ApoB is 115 (moderately elevated). He wants you to "explain what this all means."
What NOT to do:
❌ "Your HbA1c is 6.2%, which means you have prediabetes, and your inflammation is concerning, so this needs to be addressed immediately."
Why it doesn't work: You’ve diagnosed him ("you have prediabetes") and turned up the fear without giving him a clear next step or any context for what’s changeable.
What TO do:
✅ Educate generally, emphasize lifestyle connections, include referral language.
Sample dialogue:
Coach: "Thanks for sharing these. I can walk you through what these markers generally indicate, and then we'll talk about what you'll want to discuss with your doctor. Your HbA1c is 6.2%, and it reflects your average blood sugar over the past few months. Values between 5.7 and 6.4 are considered the 'prediabetes' range, which simply means blood sugar control isn't as efficient as it could be. The encouraging part is that this often responds really well to consistent lifestyle changes."
Marcus: "So I have prediabetes?"
Coach: "Your doctor would make that determination, but what I can tell you is that these values are in a range where nutrition and exercise can make a real difference, and people often see meaningful improvement when they stick with a few key habits over time. Your hsCRP is 3.8, which suggests some chronic inflammation, and there are a lot of everyday factors that can influence that number. Lifestyle factors—exercise, anti-inflammatory foods, sleep, and stress management—can help bring it down. Here's what I recommend: Schedule a follow-up with your doctor to review these results in the context of your full health picture, and then let's build a plan together based on what matters most to you. What would you like to focus on first: the nutrition side or the exercise side?"
Key takeaway: Educate without diagnosing, always include "discuss with your doctor," and focus on actionable lifestyle interventions.
[CHONK: Deep Health Assessment]
Deep Health Assessments: What Numbers Miss¶
Objective tests can tell you a lot, but they can still miss something important: how people feel. Someone can have perfect blood work and still feel exhausted and miserable, while someone else can have so-so biomarkers yet feel pretty great. That’s why you’ll want objective data and subjective data working together, so you can compare what the tests show with what the client is experiencing day to day.
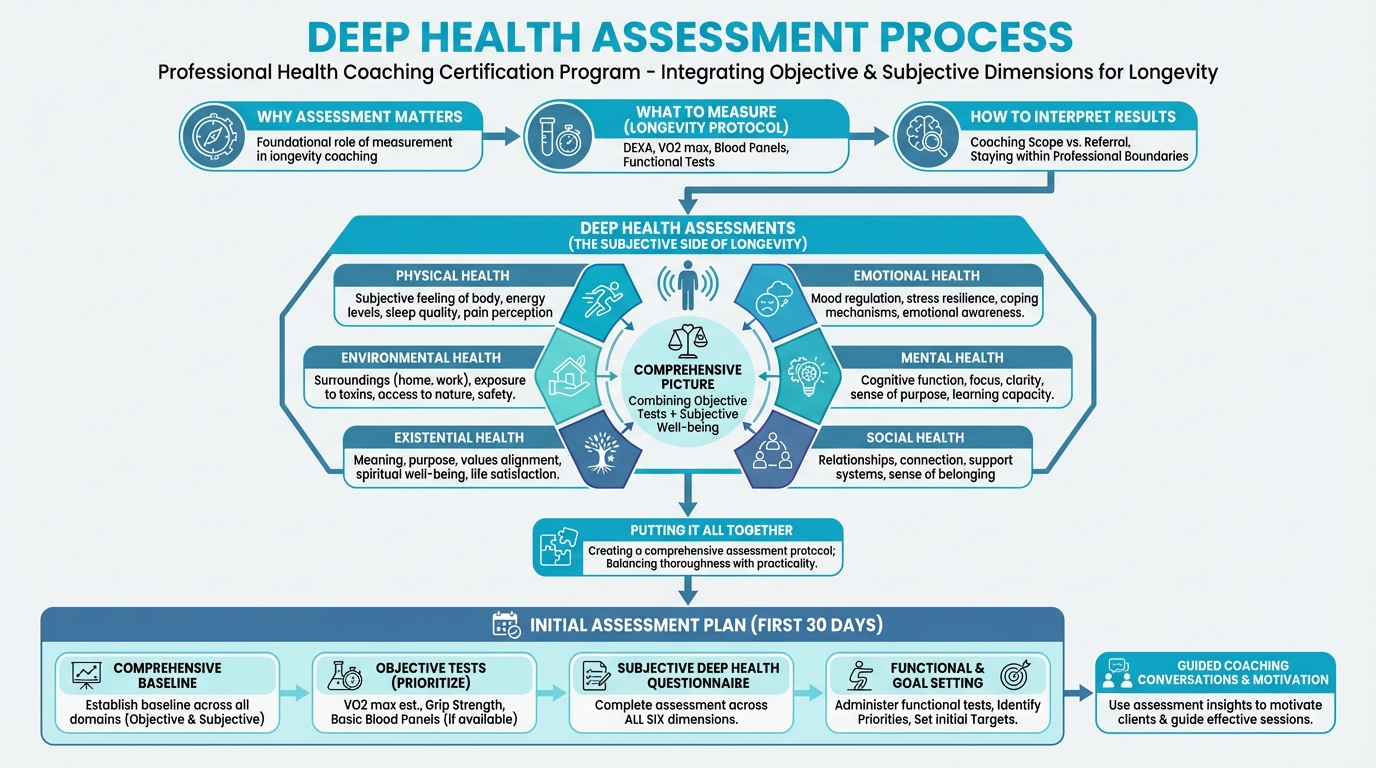
Figure: One way to conduct a 6-dimension assessment
The Six Dimensions Applied¶
In practice, you’re looking at each Deep Health dimension to get a clear picture of the client’s current state, challenges, strengths, and how this dimension connects to the others. You don’t have to get it perfect; you’re just trying to see the whole person.
Physical: Energy levels, sleep quality, pain, physical function, recovery
- "On a scale of 1-10, how would you rate your energy most days, and do you usually wake up feeling rested?"
Emotional: Stress levels, mood, emotional regulation, resilience
- "How would you describe your stress day-to-day, and how do you typically handle difficult emotions?"
Mental/Cognitive: Clarity, focus, memory, mental fatigue
- "How would you rate your mental clarity, and have you noticed any changes in memory or focus?"
Social: Relationship quality, connection, loneliness, support
- "Do you feel connected to people who matter to you, and how often do you feel lonely?"
Environmental: Living situation, access to resources, safety, nature exposure
- "Does your environment support your health goals, and do you have easy access to healthy food and places to exercise?"
Existential: Purpose, meaning, values alignment, life satisfaction
- "Do you feel like your life has purpose, and what gets you out of bed in the morning?"
Integrating Objective and Subjective¶
The real value comes from combining both, so you’re not overreacting to a lab value or ignoring what a client is living with day to day. It takes some practice to hold both at once.
Example: A client has perfect blood work but reports low energy, high stress, and loneliness. The objective tests say "healthy," yet the subjective assessment shows what’s actually driving their day-to-day experience. In that case, you’d likely focus on stress management, social connection, and sleep, rather than chasing biomarkers.
Example: A client has concerning metabolic markers but feels great. Their good subjective health doesn’t erase the objective concern, so you work on both. At the same time, feeling good suggests they may have strengths and resources to draw on as they make changes, which is helpful information to have.
The scenario: Jennifer, 47, has excellent blood work and good functional test scores, but she tells you, "I don't understand. My tests are fine, but I feel awful; I'm exhausted, stressed, and I don't know why I bother."
What NOT to do:
❌ "Well, your numbers look great! You should feel good about that."
Why it doesn't work: It dismisses her lived experience just because it doesn’t match the data.
What TO do:
✅ Take the subjective data seriously, and use Deep Health to find what the tests missed.
Sample dialogue:
Coach: "Your numbers look good, yet you feel terrible, and both of those can be true. These tests measure certain things, but they don't capture everything that matters for your day-to-day life. Can we zoom in a bit and talk about the exhaustion?"
Jennifer: "I sleep 7 hours, but I wake up tired, drag through the day, and by evening I'm useless."
Coach: "Got it, and what’s the stress been like lately?"
Jennifer: "Work is relentless. I’m managing a team through a reorg, and when I get home I just… scroll until I fall asleep."
Coach: "When you say 'why bother,' what does that feel connected to for you?"
Jennifer: "I used to love what I do, but now I'm just going through the motions. My kids are grown, my job feels meaningless, and I don't know what I'm working toward."
Coach: "Thank you for saying that out loud. So we’re looking at sleep that isn’t restorative, chronic work stress, and a sense that purpose has faded. Those won’t show up on blood tests, but they absolutely affect how you feel, and over time they can affect those numbers too. Which of these feels most important to address first?"
Key takeaway: Subjective data is data, and when numbers and feelings don’t match, take both seriously.
[CHONK: Putting It Together]
Putting It Together — Practical Assessment Protocols¶
[CHONK: Putting It Together]
Putting It Together: Practical Assessment Protocols¶
You've got a lot of possible assessments to choose from, and you do not need to use all of them to coach well. Start simple, use what's accessible, and add complexity only when it clearly helps the client move forward.
The Assessment Hierarchy¶
Think of this as a "most useful first" list. Tier 1 gives you a lot of signal with minimal cost and hassle, and then you scale up from there based on goals, access, and medical support.
Tier 1 (Essential, accessible, actionable):
- Aerobic capacity + strength basics: VO2 max estimation (Cooper test or step test), free; and grip strength, ~$30-100 for a dynamometer
- How they move + how they’re doing overall: functional movement tests, free; and the Deep Health questionnaire, free
Tier 2 (Valuable, may need medical collaboration):
- Basic blood panels (metabolic, inflammatory markers): often insurance-covered
- DEXA scan: $40-400+
Tier 3 (Advanced, limited accessibility):
- More intensive data options: full blood panels, $200-800+; and/or biological age clocks, $100-500+
- Imaging option: full body MRI, ~$2,500+
Start with Tier 1, because every client can do these regardless of budget or location. From there, build up based on access and goals, and loop in medical collaboration when needed.
Assessment Timeline¶
Here's a simple schedule you can lean on. Aim for "often enough to be useful," not "so often it becomes stressful."
Initial (first 30 days):
- Do the functional tests (VO2 max estimate, grip strength, movement tests) and the Deep Health questionnaire across all six dimensions
- Review any existing medical test results (so you’re not repeating work or spending money unnecessarily)
Ongoing:
- Keep a simple rhythm: track grip strength weekly, do a Deep Health check-in every 3 months (quarterly), and re-check the VO2 max estimate every 6 months.
- Annually (or per doctor's schedule): blood panels; plus DEXA annually for body composition and every 2-3 years for bone density
Use this as a starting template, then adjust based on the client's life, stress, and access.
Accessibility Reality Check¶
Not everyone can access everything. That’s normal, and it doesn’t disqualify someone from making meaningful progress.
Your job is to work with what clients have and help them spend their time, energy, and money where it counts most.
Limited budget: Focus on Tier 1 entirely. You can do excellent longevity coaching with just functional tests and Deep Health assessments.
Rural location: Functional tests work anywhere, while DEXA and lab access may require travel. Factor that into frequency so the plan fits real life.
Insurance gaps: Know what preventive care is covered (often basic metabolic panels). Then help clients prioritize out-of-pocket spending so they’re paying for the highest-value information first.
Coaching in practice (quick example)¶
What NOT to do:
- Default to Tier 3 testing because it feels “more thorough,” even when the client doesn’t have access, budget, or a clear reason to do it.
Better (simple, client-centered):
Client: “I keep seeing influencers talk about full-body MRIs and biological age tests. Should I do those first?”
Coach: “Totally fair question. Before we spend money there, can we start with a few Tier 1 basics that give us actionable information right away?”
Client: “Like what?”
Coach: “A VO2 max estimate, grip strength, a few movement checks, and the Deep Health questionnaire. Those are accessible and they help us decide whether any higher-tier testing would actually change what we do next.”
Client: “So the advanced tests aren’t always necessary?”
Coach: "Exactly. We can add Tier 2 or Tier 3 later if you have access and a clear goal for the data. For now, we'll focus on what you can do consistently and what will move the needle."
[CHONK: Coaching in Practice - Presenting Results]
Coaching in Practice: Presenting Mixed Results¶
The scenario: David, 59, completed his full assessment. His results are mixed, with some encouraging signs and some areas that need attention. That’s common, and it’s exactly why we assess.
Results:
- Performance: VO2 max 26 mL/kg/min (below target); grip strength 70 lbs (good)
- Blood markers: HbA1c 6.3% (prediabetic range); hsCRP 2.4 (average risk)
- Deep Health: Physical struggling (poor sleep, low energy); Social strong
What NOT to do:
❌ Lead with the concerning numbers and create alarm.
What TO do:
✅ Balance honesty with hope by highlighting both strengths and areas for improvement, then make it actionable.
Sample dialogue:
Coach: "David, thanks for going through the full assessment. Before we jump into the results, how are you feeling about all of this? It can be a lot to take in."
Client: "Honestly, I’m a little nervous, and I don’t really know what to expect."
Coach: "Totally fair, and I’m glad you said that. A lot of people feel the same way at first. Here’s what I want you to know up front: this gives us a clear picture, and we’re going to use it to make a simple, doable plan. We’ll start with what’s going well, then talk about the few areas that need attention. Sound okay?"
Client: "Yeah, that helps."
Coach: "How about we start with strengths? Your grip strength is solid at 70 pounds, which tells me your overall strength is in a good place, and that matters because strength is protective for longevity. Your Social score is strong too, which research shows is a big deal for health and lifespan."
Client: "Okay, good. So if you had to pick the main thing to work on first, what would it be?"
Coach: "The biggest opportunity is cardio fitness: your VO2 max came in at 26, and we’re aiming for 35+. VO2 max is the single strongest predictor of longevity, and it’s highly trainable, which means you’re not stuck here. With three months of consistent cardio work, we can move this, and we’ll build it in a way that fits your life."
Client: "That feels reassuring. What about the blood sugar number?"
Coach: "Your HbA1c is 6.3%, which lands in the prediabetic range, so it’s worth taking seriously. Your doctor should review this, and from a lifestyle standpoint we can support it with nutrition and exercise, since both improve insulin sensitivity."
Client: "Makes sense. And the sleep part?"
Coach: "Your Deep Health assessment flagged sleep and energy as struggles, and that lines up with what you’ve told me about feeling tired. You’re not doing anything 'wrong' here. Sleep issues are common, and improving sleep will support everything else we’re working on."
Client: "So where do we start?"
Coach: "Bottom line: we have clear priorities, and we’ll keep this simple and doable. We’ll focus on cardio fitness first, work on sleep optimization alongside it, and make nutrition adjustments that support blood sugar, all while building on the real strengths you already have. What feels like the easiest first step for you this week?"
Key takeaway: Lead with strengths, be honest about concerns, and finish with clear next steps. Avoid just dumping numbers on people.
The scenario: Robert, 56, has been working with you for 3 months. He's frustrated because he has only lost 5 pounds, but his functional metrics tell a different story.
[CHONK: Coaching in Practice - Motivating with Functional Progress]
Coaching in Practice: When the Scale Disappoints¶
The scenario: Robert, 56, has been working with you for 3 months. He's frustrated because he's only lost 5 pounds, even though his functional metrics tell a very different story.
Results:
- Baseline: Grip 55 lbs, VO2 max estimate 22, TUG 12.1 seconds
- 3 months: Grip 68 lbs, VO2 max estimate 27, TUG 9.4 seconds
Take a second to notice what’s happening here: the scale is giving Robert one story, while his body is giving him another. If he’s feeling torn between those two, that’s normal.
What NOT to do:
❌ "Well, the scale isn't everything. At least your other numbers improved."
Why it doesn't work: It brushes past his goal, and it can land like a shrug, even if you mean well.
What TO do:
✅ Reframe what "progress" means for longevity and help the functional gains feel real.
Sample dialogue:
Robert: "Five pounds in three months, and I could've done that by just eating less."
Coach: "I hear your frustration, Robert; when the scale moves slowly, it can feel like all your effort isn't paying off. Before we judge the last three months, can I show you what's actually happened in your body?"
Robert: "What do you mean?"
Coach: "Look at these changes: your grip strength went from 55 to 68 pounds (a 24% increase), your VO2 max improved from 22 to 27 (more than 20% better cardiovascular fitness), and your TUG time dropped from 12.1 to 9.4 seconds, which means you moved from the 'higher risk' zone into the normal range. Here’s why that matters: these are the metrics that actually predict how long and how well you'll live, and research shows they matter more than the number on the scale. In a very real way, you’ve gotten functionally younger in 3 months, and that counts."
Robert: "I didn't realize those numbers had changed that much, and I guess I’ve been staring at the scale."
Coach: "Totally. Most people don't track what matters, and the scale really tells you just one thing: your relationship with gravity. These tests tell you how your body functions in the real world, and right now it's functioning better than it was three months ago. The scale will likely catch up, but even if it doesn't, these improvements are real wins. You earned them."
Key takeaway: Functional metrics tell the longevity story better than scale weight, so help clients see what actually matters.
Study Guide Questions¶
If these feel challenging, that’s okay; use them to guide your thinking, not to “ace” the chapter. Questions 1–3 focus on functional capacity, 4–5 on scope and labs, and 6–10 on assessment and coaching conversations.
-
Why is VO2 max considered the strongest predictor of all-cause mortality, and what's the target for longevity?
-
What are the EWGSOP2 grip strength thresholds, and why do they matter for coaching?
-
Name three functional movement tests that predict mortality. What makes them valuable for coaches?
-
What's the difference between what coaches can say about DEXA results versus what requires medical referral?
-
How do you discuss blood panel results with clients while staying in scope? Give an example.
-
Why is Deep Health assessment important even when objective biomarkers look good?
-
What's the "assessment hierarchy" (Tier 1, 2, 3), and why should coaches prioritize Tier 1?
-
How would you respond to a client who says "I don't want to know my numbers"?
-
A client's scale hasn't moved much, but their functional tests improved significantly. How do you reframe this?
-
What's the difference between screening (what coaches do) and diagnosis (what doctors do)?
Self-reflection questions:
-
Think about your own functional markers: How quickly can you get up from the floor, how long can you hang from a bar, and can you easily stand from a chair without using your hands? What might those answers tell you about your own aging trajectory?
-
When was your last physical exam or bloodwork, and what conversations might you want to have with your healthcare provider about longevity-relevant markers? (No need to overthink it; just notice what comes up.)
Want more detail? These supplemental articles explore key topics from this chapter in a bit more depth.
- Understanding Blood Panels for Coaches : Non-diagnostic interpretation guidance
- VO2 Max: The Ultimate Longevity Biomarker : Why it matters and how to improve it
- Biological Age Clocks: What Coaches Need to Know: The promise, limitations, and how to discuss with clients
References¶
-
Lang JJ, Tomkinson GR, Janssen I, et al. Cardiorespiratory fitness as a predictor of mortality: an overview of meta-analyses. British Journal of Sports Medicine. 2024;58:595-609. doi:10.1136/bjsports-2023-107731
-
Lang JJ, et al. Mortality risk reduction by cardiorespiratory fitness level, British Journal of Sports Medicine, 2024.
-
Huang W, et al. Dose-response meta-analysis of cardiorespiratory fitness and mortality. British Journal of Sports Medicine. 2022. doi:10.1136/bjsports-2021-104377
-
López-Bueno R, Andersen LL, Calatayud J, et al. Associations of handgrip strength with all-cause and cancer mortality in older adults: a prospective cohort study in 28 countries. Age and Ageing. 2022;51(5). doi:10.1093/ageing/afac117
-
Oksuzyan A, Demakakos P, Shkolnikova M, et al. Handgrip strength and its prognostic value for mortality in Moscow, Denmark, and England. PLOS ONE. 2017;12(9):e0182684. doi:10.1371/journal.pone.0182684
-
de Brito LBB, Ricardo DR, de Araújo DSMS, et al. Ability to sit and rise from the floor as a predictor of all-cause mortality. European Journal of Preventive Cardiology. 2012;21(7):892-898. doi:10.1177/2047487312471759
-
Cheong CY, Yap P, Gwee X, et al. Physical and functional measures predicting long-term mortality in community-dwelling older adults. Aging. 2021;13(23):25038-25054. doi:10.18632/aging.203756
-
Nude T, et al. Gait speed and all-cause mortality: A systematic review and meta-analysis, European Geriatric Medicine, 2018.
-
American College of Physicians. Balance (10-second One-Legged Stance) and Mortality, I.M. Matters Weekly, 2022.
-
Cruz-Jentoft AJ, Bahat G, Bauer J, et al. Sarcopenia: revised European consensus on definition and diagnosis. Age and Ageing. 2019;48(4):601. doi:10.1093/ageing/afz046
-
Gierisch JM, et al. Health Coaching. Comparative Effectiveness Review No. 195. AHRQ. 2017.
-
Holt-Lunstad J, Smith TB, Layton JB. Social Relationships and Mortality Risk: A Meta-analytic Review. PLoS Medicine. 2010;7(7):e1000316. doi:10.1371/journal.pmed.1000316
-
Alimujiang A, Wiensch A, Boss J, et al. Association Between Life Purpose and Mortality Among US Adults Older Than 50 Years. JAMA Network Open. 2019;2(5):e194270. doi:10.1001/jamanetworkopen.2019.4270
Chapter 1.4 complete. Proceed to Chapter 1.5: Scope of Practice and Medical Collaboration.