Unit 2: Core Interventions (The Protocol)¶
Chapter 2.7: Nutrition for Longevity¶
[CHONK: 1-minute summary]
What you'll learn in this chapter:
- How food affects aging biology through nutrient-sensing pathways (mTOR, AMPK, sirtuins)
- The Mediterranean and MIND dietary patterns: what they are, and why they work
- Protein requirements for preventing muscle loss (sarcopenia) as we age
- Practical targets for fiber and vegetable intake
- Evidence-based guidance on what to limit (ultra-processed foods, alcohol)
- How to discuss nutrition within your coaching scope
- A sample day showing these principles in action
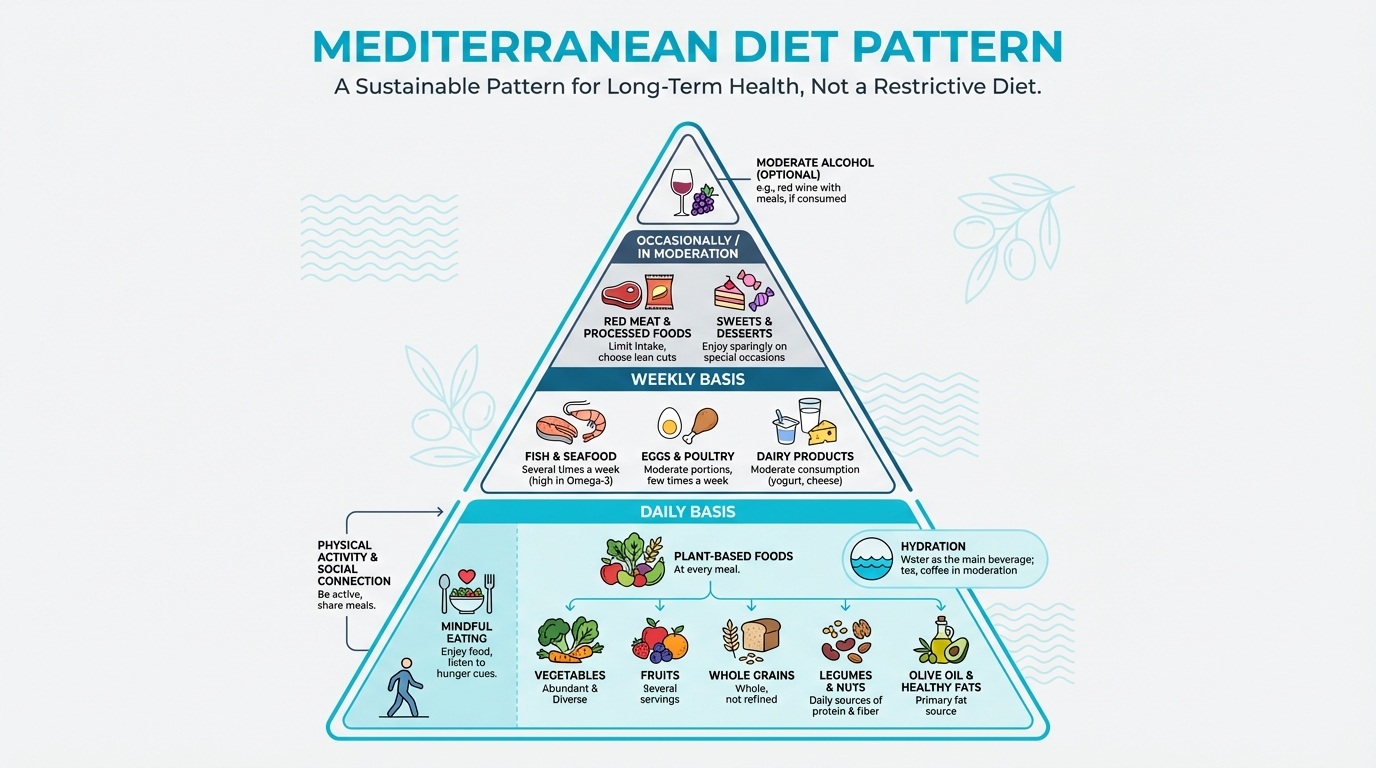
Figure: Visual representation of food groups, portions, frequencies
The big idea: Nutrition for longevity isn't about restriction or perfection. It's about consistently eating in ways that support your body's maintenance and repair systems. The research points clearly to a Mediterranean-style approach, adequate protein, abundant plants, and minimizing ultra-processed foods. This chapter gives you the evidence, the practical targets, and a coaching approach to help clients eat for a longer, healthier life.
Coaching in action (quick example):
What not to do
- Coach: “You need to follow the Mediterranean diet perfectly starting today.”
Try this instead
- Client: “Do I need a special diet to live longer?”
- Coach: “Not a perfect one. Would you be open to starting with one change that supports your health span, like adding a serving of vegetables at lunch?”
- Client: “Yeah, that feels doable.”
- Coach: “Great. We’ll build from there, and I’ll stay within my scope by focusing on food patterns and habits you can actually stick with.”
[CHONK: Introduction: Why Nutrition for Longevity Is Different]
Introduction: More Than "Healthy Eating"¶
You probably already know that nutrition matters. But coaching nutrition for longevity is different from coaching for weight loss or performance. Here, we're playing a longer game, decades, not weeks.
When clients come to you wanting to "eat for longevity," they're asking a deeper question: How do I eat in a way that supports my body's ability to maintain itself, repair damage, and stay functional as I age?
That question connects directly to the biology you learned in Chapter 1.2. Remember the hallmarks of aging? Several of them—nutrient sensing, autophagy, mitochondrial function, inflammation—are directly influenced by what and how much you eat.
This isn't about finding the "perfect diet." It's about understanding which eating patterns consistently show up in longevity research, and helping clients build sustainable habits around those patterns.
What This Chapter Covers¶
We'll cover the what of eating for longevity:
- Which dietary patterns have the strongest evidence
- How much protein older adults need (it's more than you might think)
- Why fiber and plant diversity matter
- What to reduce and why
We won't cover when to eat. That's Chapter 2.8 (Metabolic Health & Nutrition Timing), where we'll discuss meal timing, time-restricted eating, and metabolic flexibility.
The Hierarchy: Essential → Valuable → Optional¶
Not all nutrition interventions are equal. Here's how to think about priorities:
Essential (focus here first):
- Adequate protein (prevents muscle loss)
- Abundant vegetables and fiber
- Minimizing ultra-processed foods
Valuable (add once essentials are solid):
- Mediterranean/MIND dietary pattern
- Omega-3 rich foods or supplementation
- Diverse plant foods for microbiome health
Optional (fine-tuning for those with fundamentals dialed):
- Specific supplements beyond basics
- Advanced meal composition strategies
- Precise macronutrient ratios
This hierarchy matters. Don't let clients obsess over omega-3 timing if they're eating processed food for most meals.
[CHONK: How Food Affects Aging Biology]
How Food Affects Aging Biology¶
Your cells have two basic modes: build mode and repair mode.
When you eat (especially protein), your cells shift into build mode and focus on growth. When you haven't eaten for a while, your cells shift into repair mode and focus on maintenance and cleanup.
Both modes are necessary: build mode maintains muscle, while repair mode cleans up cellular damage. The problem is when you're always in build mode, eating constantly and never giving your cells time to do maintenance.
Why This Matters for Longevity¶
As we age, we tend to get stuck in build mode, with our cells continuing to prioritize growth when they should be repairing. This is one reason chronic overeating, even of healthy foods, may accelerate aging at the cellular level.
The research is striking: animals with reduced "build mode" signaling live significantly longer.
The Practical Takeaway¶
You don't need to understand the biochemistry to coach effectively, because you can get a lot of results by focusing on a few simple basics. (This is actually simpler than it sounds.)
- Eat adequate protein at meals to help maintain muscle
- Don't eat constantly; allow time between meals so your body can spend more time in repair mode
- Chronic overeating accelerates aging, regardless of food quality
That's why what you eat and how much both matter for longevity.
Coaching example¶
What NOT to do
Coach: “You need to inhibit mTOR and activate AMPK.”
Client: “I’m not really sure what that means.”
Better
Client: “So should I just eat less all the time to stay in repair mode?”
Coach: “Not necessarily; a good place to start is adequate protein at meals, and then we can build in some time between meals so your body can spend more time in repair mode.”
For the full biochemistry (mTOR, AMPK, sirtuins), see More detail: How Food Affects Aging Biology.
[CHONK: The Mediterranean and MIND Approach]
The Mediterranean and MIND Approach¶
Spend any time in longevity research and you’ll see one dietary pattern come up again and again: the Mediterranean diet. It’s not the only healthy way to eat, but it has the strongest evidence base for longevity outcomes.
Why a Dietary Pattern, Not a “Diet”¶
Here, we're talking about a pattern of eating, not a restrictive diet with forbidden foods. The Mediterranean approach describes what people in Mediterranean regions traditionally ate, rather than a commercial program with rules and phases. In other words, no "day 1, day 7, day 30" checklist required.
Why this matters:
- No single diet works for everyone. Cultural background, food access, preferences, and health conditions all affect what’s realistic.
- Patterns are sustainable; restrictions aren’t, which means clients can adopt Mediterranean principles while still eating foods they love.
- The whole pattern matters more than individual foods. No single “superfood” drives the benefits; it’s the combination.
If you’re thinking, “Okay, but my client’s life is complicated,” you’re right. That’s normal, and it’s exactly why patterns tend to work better than rigid rules.
What Is the Mediterranean Diet?¶
The Mediterranean dietary pattern emphasizes:
- Vegetables in abundance: 6-10 servings daily, aiming for variety and color across the week
- Fruits: Especially berries and other whole fruits (fresh or frozen both work)
- Whole grains: Bread, pasta, rice, and other grains, choosing minimally processed versions most often
- Legumes: Beans, lentils, chickpeas, and similar staples that add protein and fiber
- Nuts and seeds: Especially almonds, walnuts, and seeds, in small portions most days
- Olive oil: As the primary added fat source, especially extra-virgin when you can
- Fish and seafood: 2-3 times weekly, with an emphasis on fatty fish
- Moderate dairy: Cheese and yogurt in moderation, depending on preference and tolerance
- Limited red meat: A few times monthly rather than daily
- Moderate wine: Traditionally included, though we’ll discuss alcohol separately
The Evidence for Longevity¶
The evidence is strong, and it shows up in long-term cohort studies, randomized trials, and meta-analyses:
The Women’s Health Study followed over 25,000 U.S. women for approximately 25 years. Those with the highest Mediterranean diet adherence had 23 percent lower all-cause mortality compared to those with lowest adherence (JAMA Network Open, 2024).
Randomized trial evidence points the same way. PREDIMED, a landmark randomized trial of nearly 7,500 high-risk adults, found that those assigned to a Mediterranean diet supplemented with extra-virgin olive oil or nuts had about 30 percent fewer major cardiovascular events (heart attacks, strokes, cardiovascular deaths) compared to a low-fat control group over roughly five years (NEJM, 2013; Advances in Nutrition, 2014).
And when researchers pool data, the trend holds. Meta-analyses across 29 cohorts showed a linear, dose-response relationship: the more closely people followed Mediterranean principles, the lower their mortality risk. Even modest increases in adherence conferred benefits (Advances in Nutrition, 2019). So this isn’t an all-or-nothing approach.
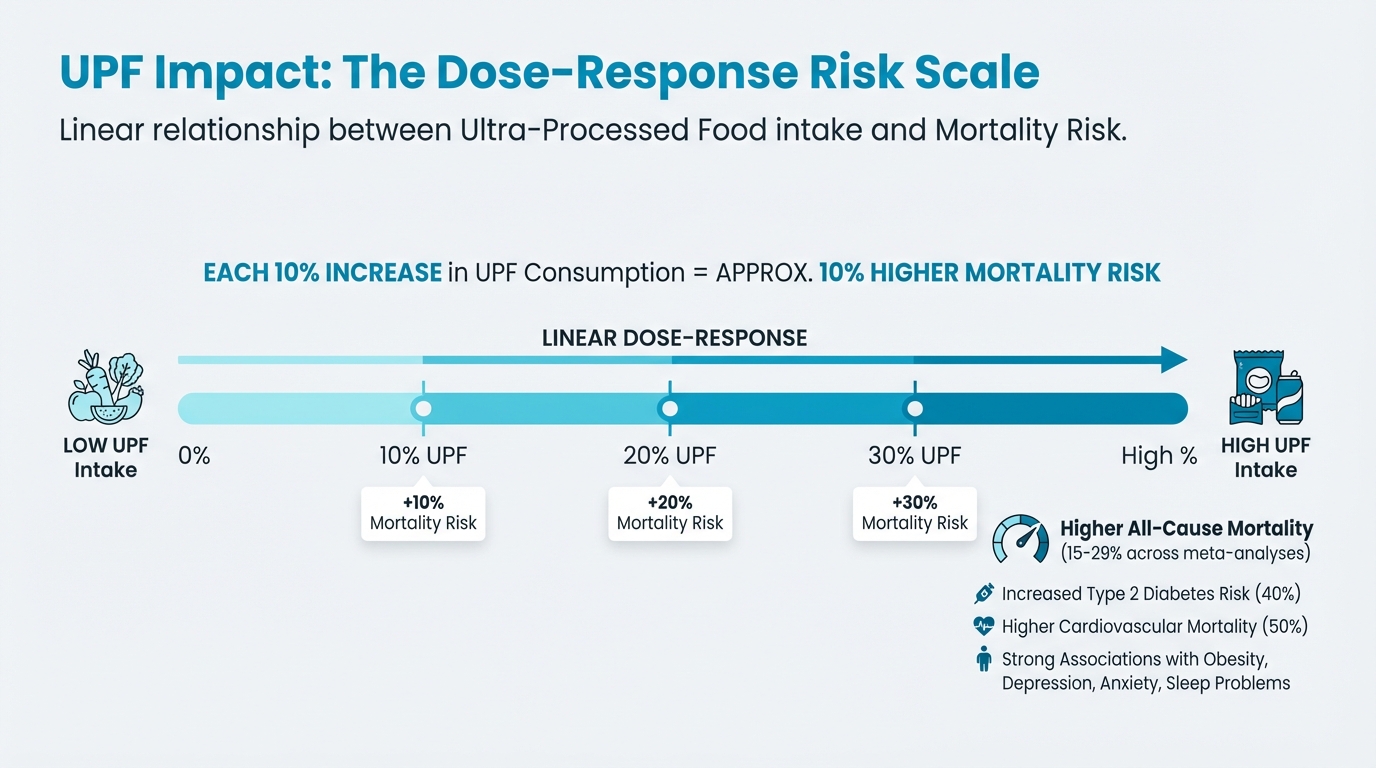
Figure: Dose-response relationship (10% increase = 10% mortality)
Mechanisms: The benefits appear to work through reduced inflammation, improved lipid profiles (cholesterol), lower insulin resistance, better body composition, and even slower epigenetic aging. One trial found that higher Mediterranean adherence reduced “epigenetic age acceleration” by approximately 1.4 years (Nutrients, 2024).
If the mechanisms list feels like a lot, that’s okay. You don’t have to “teach” inflammation or epigenetics to help someone eat more vegetables, beans, and olive oil. The basics still matter most.
The MIND Diet: Mediterranean Meets Brain Health¶
The MIND diet (Mediterranean-DASH Intervention for Neurodegenerative Delay) was specifically designed to support cognitive health. It combines elements of the Mediterranean and DASH (Dietary Approaches to Stop Hypertension) diets, with emphasis on foods linked to brain health.
Brain-healthy foods emphasized:
- Leafy green vegetables (at least 6 servings weekly), plus other vegetables (at least 1 daily)
- Berries (at least 2 servings weekly) and nuts (5+ servings weekly)
- Olive oil (as primary cooking fat) and whole grains (3+ servings daily)
- Fish (at least 1 weekly), beans (4+ meals weekly), and poultry (2+ meals weekly)
Foods to limit:
- Red meat (fewer than 4 servings weekly) and fried/fast food (fewer than 1 weekly)
- Butter/margarine (less than 1 tablespoon daily) and cheese (less than 1 serving weekly)
- Pastries and sweets (fewer than 5 weekly)
The evidence for cognition: In a 2025 systematic review of 18 studies, 16 reported cognitive benefits with higher MIND adherence, particularly for global cognition, memory, and executive function (Journal of Nutrition, Health & Aging, 2025). The Rotterdam Study found 15-24 percent lower dementia risk with higher MIND scores over 5-7 years (Alzheimer’s Research & Therapy, 2022).
Neuropathology studies add biological plausibility: higher MIND adherence is associated with lower odds of hippocampal sclerosis and neuronal loss at autopsy (JAMA Network Open, 2025).
And if a client is worried about “brain fog” or dementia risk, this can be a hopeful place to start: small, repeatable food choices that add up over time. No perfection required.
Practical Implementation¶
So how do you help clients actually eat this way, in real life, with real schedules and real budgets?
Start with addition, not restriction:
- Try questions like: “What vegetables could you add to dinner this week?”, “Could you try fish once or twice instead of your usual protein?”, or “What if you switched to olive oil for cooking?”
Cultural adaptation matters:
- Mediterranean principles work across cuisines. Asian, Latin American, and African food traditions can all align with these principles.
- The goal is the pattern: vegetables, legumes, fish, olive oil, whole grains, not specific Greek or Italian dishes.
Make it practical:
- Canned beans count, and so do frozen vegetables and bottled olive oil.
- Aim for consistency over perfection.
What not to do (too rigid):
Coach: “The Mediterranean diet has a lot of benefits, so I want you to follow it really closely starting tomorrow. No red meat, no sweets, and avoid processed foods.”
Client: “That feels pretty impossible with my schedule.”
Coach: “I hear you, but the plan works best if you stick to it exactly.”
| Coaching in Practice | |
|---|---|
| Mediterranean principles (conversation starter) Coach: “When you look at a typical week, what feels like the easiest place to start: adding a couple servings of veggies, or switching your cooking fat to olive oil?” Client: “Probably the oil. That feels doable.” Coach: “Perfect. We can start there. We’re not taking anything away right now; we’re just adding one change that research consistently links to long-term health.” |
| Coaching in Practice | |
|---|---|
| Common client objection: “I don’t like Mediterranean food” Client: “I don’t like Mediterranean food.” Coach: “Totally fair. Mediterranean eating isn’t about specific dishes like falafel or Greek salads.” Client: “So what is it then?” Coach: “More vegetables, olive oil instead of butter, fish a couple times a week, beans and lentils, and nuts for snacks. You can do that in pretty much any cuisine. What foods do you already enjoy that could fit those principles?” Client: “I like stir-fries and tacos.” Coach: “Great. We can build Mediterranean-style choices into those.” |
| Coaching in Practice | |
|---|---|
| Practical grocery list for Mediterranean principles Client: “This sounds healthy, but I’m overwhelmed.” Coach: “That makes sense. We can keep it simple. If you had just a few staples on hand, this style of eating gets much easier.” Coach: “How about we start with: extra-virgin olive oil (primary cooking fat), canned chickpeas and beans, frozen vegetables, nuts (walnuts, almonds), canned or frozen fish (salmon, sardines), whole grains (quinoa, brown rice, whole wheat pasta), and fresh or frozen berries.” Client: “Those feel manageable.” |
What This Means for Your Client¶
When you recommend Mediterranean principles, you’re not just handing out generic diet advice. You’re helping clients build an eating pattern with decades of research behind it, showing reduced mortality, cardiovascular protection, and cognitive benefits.
The evidence is strong enough that you can say, with confidence: “This is what the research consistently shows works for long-term health.” And if a client can only start with one or two changes, that’s still a meaningful step in the right direction.
[CHONK: Protein for Longevity: Preventing Sarcopenia]
Protein for Longevity: Keeping Muscle as You Age¶
Here’s a number that tends to land: By age 80, many people have lost 30-40 percent of their muscle mass. This condition, called sarcopenia, is a major driver of frailty, falls, and loss of independence.
The good news is that it's largely preventable with adequate protein and resistance training.
Why Muscle Matters¶
Muscle isn’t just for athletes; it plays a big role in day-to-day health and function:
- It helps regulate blood sugar, since muscle is where glucose goes after meals
- It provides reserves during illness (your body draws on muscle for recovery)
- It predicts independence (grip strength predicts fall risk and mortality)
The Practical Targets¶
If numbers make your eyes glaze over, you don’t need perfect tracking to get this right; a few simple targets are enough. Here’s what matters most:
A palm-sized portion of protein at each meal. That’s roughly 25-35 grams, which is generally enough to “tell” your muscles to maintain themselves. For muscle protein synthesis, each meal should also contain about 2-3 grams of leucine, the amino acid that signals muscles to build. Most animal proteins naturally provide this when you hit 25-30g of total protein; plant-based eaters need to be a bit more strategic (see below).
Breakfast is the biggest opportunity. Most people eat almost no protein at breakfast (coffee and toast, maybe 10 grams), which means it’s often the longest gap since eating and exactly when muscles could benefit. Adding eggs, Greek yogurt, or cottage cheese to breakfast is one of the highest-impact changes you can recommend. It’s a small change with a big payoff.
Spread it across the day. Eating 80 grams at dinner isn’t as effective as eating 30 grams at three meals, because your muscles can only use so much at once.

Figure: Protein distributed across meals works better than loading it all at dinner
Plant-Based? You'll Need a Bit More¶
Plant proteins work fine, but you’ll typically need larger portions to get the same muscle-building signal. Prioritize soy (tofu, tempeh, edamame) and combine proteins (beans + grains). A plant-based client might need a slightly larger palm-sized portion at each meal. It’s doable, but it takes a little more planning.
For the detailed research (g/kg requirements, leucine thresholds, anabolic resistance), see Protein Requirements Research.
What This Means for Coaching¶
| Coaching in Practice | |
|---|---|
| Protein tracking without obsession | What NOT to do: “You need to log everything you eat forever.” That tends to backfire. Try this instead (simple + effective): Coach: “To keep this practical, aim for a palm-sized portion of protein at each meal (about 25-30g), and make sure breakfast includes real protein, not just carbs.” Client: “Do I have to track it?” Coach: “Not unless you want to. If you like precision, we can track for 3-5 days to spot patterns, then go back to estimating.” |
| Coaching in Practice | |
|---|---|
| The “protein audit” conversation | What NOT to do: “You’re not eating enough protein,” followed by a lecture. Try this instead (quick, collaborative, and usually eye-opening): Coach: “Would you be up for a quick protein audit, where you walk me through what you ate yesterday for breakfast, lunch, dinner, and any snacks?” Client: “Sure, I can do that: breakfast was coffee and toast, lunch was a salad with chicken, and dinner was pasta and some meat sauce.” Coach: “Got it. If I roughly estimate that, breakfast might be 5-15g, lunch maybe 15-25g, and dinner could be 40-50g. That pattern is incredibly common, so you’re not alone. The biggest opportunity is usually breakfast, and if we bring that up, the whole day gets easier.” |
| Coaching in Practice | |
|---|---|
| Addressing the “I’m not hungry for breakfast” client | What NOT to do: “You have to eat a big breakfast,” or assuming it’s a motivation problem. Try this instead (curious + gradual): Coach: “When you say you’re not hungry in the morning, is that more habit, time pressure, or do you truly feel no appetite?” Client: “Honestly, I just don’t feel like eating.” Coach: “That makes sense. We can start small, because even 15-20 grams is better than zero. Would something like Greek yogurt or a couple of eggs feel manageable?” Client: “Yeah, I could do yogurt.” Coach: “Perfect. Your morning appetite often increases once you establish the habit, and we can build up to 30+ grams over a few weeks.” |
What About Plant-Based Clients?¶
Plant-based eating is entirely compatible with adequate protein for longevity, but it requires more intentionality:
Leucine content matters: Plant proteins generally contain less leucine per gram of protein. To hit the leucine threshold, plant-based clients need larger protein portions or strategic combinations.
Best plant protein sources for leucine:
- Soy products (tofu, tempeh, edamame): highest plant leucine content
- Legumes combined with grains
- Seitan (wheat gluten)
- Quinoa (complete protein)
Practical approach: A plant-based client might need 40-50g of plant protein per meal to achieve the same muscle protein synthesis stimulus as 30g of animal protein. This is achievable, but it does take a bit of planning. Once clients have a few go-to meals, it usually gets much easier.
| For DIY Learners |
|---|
| Applying this to yourself: Do a quick protein audit of your own typical day. Walk through yesterday: What did you eat for breakfast? How much protein was in it? What about lunch and dinner? Most people discover the same pattern: almost nothing at breakfast, light at lunch, heavy at dinner. If that's you, try adding just 20 grams to breakfast this week: Greek yogurt, eggs, or a protein shake. It's one of the highest-impact nutrition changes for longevity. |
[CHONK: Fiber, Plants, and the Microbiome]
Fiber, Plants, and the Microbiome¶
If protein is about maintaining structure, fiber and plant diversity are about maintaining systems, particularly your gut microbiome and the inflammatory environment throughout your body.
Fiber Targets: 30-50 Grams Daily¶
Most people don't come close. The average American consumes about 15 grams of fiber daily, half the minimum recommendation and far below the 30-50 grams associated with optimal health outcomes.
Why fiber matters for longevity:
- Feeds beneficial gut bacteria that produce short-chain fatty acids (SCFAs), which reduce inflammation and support gut barrier function
- Lowers cholesterol by binding bile acids
- Improves blood sugar control by slowing digestion
- Promotes regular elimination and reduces colon cancer risk
The 6-10 Servings Guideline¶
The protocol recommends 6-10 servings of colorful vegetables daily. That sounds like a lot, but a "serving" is about half a cup cooked or one cup raw.
Why color diversity matters:
Different colors indicate different phytonutrients: plant compounds with antioxidant and anti-inflammatory effects:
- Reds (tomatoes, red peppers): lycopene
- Oranges (carrots, sweet potatoes): beta-carotene
- Greens (leafy vegetables, broccoli): folate, vitamin K
- Purples/blues (berries, eggplant): anthocyanins
- Whites (garlic, onions): allicin
The goal isn't perfection, it's diversity. Different plant compounds feed different microbial populations, and microbiome diversity is associated with better health outcomes.
The Microbiome Connection¶
Your gut houses trillions of bacteria that influence:
- Inflammation throughout your body
- Immune function
- Neurotransmitter production (gut-brain axis)
- Nutrient absorption
- Even your weight regulation
A fiber-rich, plant-diverse diet promotes a healthy microbiome. Ultra-processed foods, antibiotics, and low-fiber diets do the opposite.
Practical Strategies¶
Add, don't restrict:
- Add a side salad to lunch
- Include vegetables with breakfast (spinach in eggs, tomatoes alongside)
- Keep frozen vegetables for easy additions
- Add beans to soups, salads, and grain dishes
Increase gradually:
- Rapid fiber increases cause bloating and gas
- Add 5 grams per week until reaching target
- Drink adequate water as fiber increases
Prioritize diversity over perfection:
- Aim for 30 different plant foods weekly (this sounds like a lot, but includes vegetables, fruits, whole grains, legumes, nuts, seeds, herbs, and spices)
- Variety matters more than hitting exact targets
| Coaching in Practice | |
|---|---|
| Fiber gradual increase protocol: "Rather than overhauling your diet overnight, let's add fiber gradually. This week, could you add one extra serving of vegetables to your day, maybe a side salad at lunch or an extra handful of vegetables at dinner? Next week, we'll add another. Your gut bacteria need time to adjust, and going slow prevents the bloating that makes people quit." |
The "30 Different Plants" Challenge¶
Research on the microbiome suggests that diversity matters as much as quantity. A landmark study from the American Gut Project found that people who ate 30 or more different plant foods per week had more diverse gut microbiomes than those who ate fewer than 10.
What counts as a "plant food":
- Vegetables (each type counts separately, spinach and kale are two plants)
- Fruits
- Whole grains (oats, rice, quinoa each count)
- Legumes (chickpeas, black beans, lentils each count)
- Nuts and seeds (almonds, walnuts, chia seeds each count)
- Herbs and spices (yes, basil, oregano, and turmeric count!)
When you include herbs and spices, hitting 30 plants weekly becomes much more achievable. This is a great reframe for clients who feel overwhelmed: "You're probably already eating more plant diversity than you realize. Let's count it up."
| Coaching in Practice | |
|---|---|
| The diversity conversation: "Here's something interesting from the research: eating a variety of plants matters as much as the total amount. Different plants feed different gut bacteria, and diversity in your microbiome is linked to better health. The target is about 30 different plant foods per week. That sounds like a lot, but when you count herbs and spices—basil counts, turmeric counts—you're probably closer than you think. Want to try tracking it for a week just to see where you are?" |
Why Clients Struggle With Vegetables¶
Understanding barriers helps you coach more effectively:
Taste preferences: Many adults grew up with overcooked, unseasoned vegetables. Help them discover that roasted vegetables with olive oil and salt taste dramatically different from boiled broccoli.
Convenience: Vegetables require washing, chopping, and cooking. Frozen vegetables, pre-cut options, and roasting large batches help.
Habit: If someone has eaten the same meals for years, vegetables feel like an addition rather than a default. Building new routines takes time.
Cost perception: Fresh vegetables can seem expensive. Frozen vegetables, canned beans, and seasonal produce are affordable alternatives with equivalent nutrition.
[CHONK: What to Limit: Evidence-Based Guidance]
What to Limit: Evidence-Based Guidance¶
Longevity nutrition isn't just about what to add. There are also foods and substances worth reducing. The key is presenting this honestly without creating food fear or orthorexic anxiety.
Ultra-Processed Foods (UPFs)¶
What they are: The NOVA classification defines ultra-processed foods as industrial formulations made mostly from substances derived from foods plus additives. Think: packaged snacks, sweetened beverages, instant noodles, many breakfast cereals, reconstituted meat products.
The evidence is substantial:
- Highest vs. lowest UPF intake is associated with 15-29 percent higher all-cause mortality across multiple meta-analyses (Liang et al., 2025; American Journal of Epidemiology, 2022)
- 40 percent higher type 2 diabetes risk (Frontiers in Nutrition, 2024)
- 50 percent higher cardiovascular mortality with convincing evidence (BMJ umbrella review, 2024)
- Strong associations with obesity, depression, anxiety, and sleep problems
Not all UPFs are equal:
- Processed meats and sugar-sweetened beverages show the strongest harmful associations
- Some UPF categories (like certain fortified breakfast cereals) show neutral or even inverse associations
- The dose-response is linear: each 10 percent increase in UPF consumption is linked to approximately 10 percent higher mortality risk
The coaching approach:
- Focus on reduction, not elimination. Perfection isn't the goal
- Help clients identify their highest-impact swaps (replacing daily soda has more impact than worrying about occasional packaged crackers)
- Emphasize adding whole foods, which naturally displaces UPFs
Added Sugars and Sugar-Sweetened Beverages¶
Sugar-sweetened beverages are the single most consistently harmful category in nutrition research. They provide calories without satiation, spike blood sugar, and are associated with metabolic disease risk.
Practical targets:
- Limit added sugars to less than 10 percent of calories (about 50 grams for a 2,000-calorie diet)
- Replace sweetened beverages with water, unsweetened tea/coffee, or sparkling water
- Read labels. Sugar hides in sauces, dressings, and "healthy" packaged foods
Saturated Fat: Context Matters¶
The recommendation to keep saturated fat below 10 percent of calories is based on its effects on LDL cholesterol and cardiovascular risk. But context matters:
- Quality matters: Saturated fat from whole foods (eggs, full-fat dairy) appears less harmful than from processed foods
- Replacement matters: Replacing saturated fat with refined carbohydrates doesn't improve outcomes; replacing with unsaturated fats (olive oil, nuts, fish) does
- Individual variation exists: Some people's cholesterol responds more to dietary saturated fat than others
The practical approach:
- Use olive oil as primary cooking fat
- Don't obsess over every gram of saturated fat
- If cardiovascular risk is elevated (high ApoB), saturated fat reduction becomes more important
Avoiding Food Fear¶
Here's the challenge: too much focus on "bad" foods creates anxiety that may be worse than the foods themselves.
The 80/20 principle:
- If 80 percent of someone's diet consists of whole, minimally processed foods, the other 20 percent matters much less
- Occasional pizza, birthday cake, or restaurant meals don't derail longevity
- Social eating and food enjoyment are part of Deep Health
Language matters:
- "Foods to eat less often" rather than "bad foods"
- "Let's focus on adding these foods" rather than "you need to eliminate these"
- "How does eating this way make you feel?" rather than "this food is toxic"
| Coaching in Practice | |
|---|---|
| The "swap" conversation instead of "eliminate": "I notice you're eating packaged granola bars as snacks most days. Those are pretty processed: lots of added sugar and not much protein. What if we experimented with some alternatives? A handful of nuts and an apple? Greek yogurt? You don't have to give up the granola bars entirely, but what if they became the backup option instead of the default?" |
Identifying High-Impact Swaps¶
Not all UPF reduction is equal. Focus coaching on the highest-impact changes:
High impact (worth prioritizing):
- Sugar-sweetened beverages → water, unsweetened tea, sparkling water
- Processed meats (daily) → fish, poultry, legumes
- Packaged snacks → nuts, vegetables, whole fruit
- Sweetened breakfast cereals → oatmeal, eggs, Greek yogurt
Lower impact (don't obsess):
- Occasional condiments with added sugar
- Whole grain bread (technically processed, but beneficial)
- Plain crackers with whole food toppings
Help clients distinguish between "ultra-processed" and "any processing." All cooking is processing. The concern is industrial formulations designed for hyper-palatability, not foods that simply come in packages.
[CHONK: Alcohol: The Honest Conversation]
Alcohol: The Evidence Coaches Need to Know¶
Alcohol gets its own section because the science has shifted a lot in the last few years. As a coach, you want clear, current info so you can talk with clients in a way that’s honest and non-judgy.
The Old Story vs. The New Evidence¶
The old story (what many clients believe): Moderate drinking, especially red wine, is good for your heart. The "J-curve" suggested that moderate drinkers lived longer than abstainers.
The new evidence (what research now shows): When researchers controlled for biases in those earlier studies, the apparent protective effect mostly disappeared. This surprised a lot of people.
A 2023 meta-analysis in JAMA Network Open pooled 107 cohort studies (4.84 million participants) and found:
- No statistically significant mortality benefit for low-to-moderate drinking compared to lifetime abstainers
- Occasional drinkers (<1.3 g/day): RR 0.96 (95% CI 0.86–1.06). Not significant
- Low-volume drinkers (1.3–24 g/day): RR 0.93 (P=0.07). Not significant
- Higher consumption increased mortality (45–64 g/day: RR 1.19; ≥65 g/day: RR 1.35)
(Zhao et al., 2023, JAMA Network Open)
Why the J-Curve Was Wrong¶
That apparent "protection" from moderate drinking wasn’t magic. It mostly came down to a few study-design issues that made moderate drinkers look healthier than they actually were, at least on paper:
Sick quitter bias: Many "abstainers" in studies were former drinkers who quit due to health problems. Comparing current moderate drinkers to this less healthy group made drinkers look healthier.
Healthy user bias: Moderate drinkers tend to be wealthier, more educated, and have healthier lifestyles overall, so the apparent "benefit" may have been confounded by those factors.
Mendelian randomization (using genetic variants as natural experiments) does not confirm cardiovascular benefits from moderate drinking (Tsai & Gao, 2023, BMC Medicine).
If you’re thinking, “Wait, so what do I tell clients who’ve heard wine is heart-healthy?” you’re not alone. This is exactly why we’re updating the story, even if it can feel a little whiplashy.
The Cancer Issue¶
Even if cardiovascular effects are still debated, the cancer data are much clearer, so we don’t have to guess here.
There is no safe level of alcohol for cancer risk. Even very moderate intake increases risk for:
- Breast cancer
- Oral and throat cancers
- Esophageal cancer
- Colorectal cancer
If reading that makes you feel uneasy, that’s normal; it’s a lot to take in, and it often bumps into culture, family habits, and social life.
The WHO Regional Office for Europe states explicitly: "There is no safe amount of alcohol that does not affect health" (WHO, 2023).
The National Academies of Sciences, Engineering, and Medicine (NASEM) 2025 report concludes: "Drinking less is better than drinking more" and advises not to start drinking for health benefits.
How to Talk About This With Clients¶
This is where coaching skill really shows up: you’re not the alcohol police, and prohibition-style messaging often backfires. What helps is having a simple, practical way to talk it through. You don’t need to “win” this topic. You just need to support an informed choice.
For coaches (what you need to understand):
- The evidence no longer supports "moderate drinking is healthy"
- Any amount increases cancer risk
- The "tolerable risk" is low. The protocol suggests 0-4 drinks/week maximum, with less being better
- Some people will choose to drink despite the risks, and that's their choice to make
Coaching in Practice: “Is it okay to have a glass of wine with dinner?”¶
What not to do (examples):
- “Red wine is good for your heart, so you’re fine.”
- “No. Alcohol is poison. Stop drinking.”
A balanced, real-life dialogue:
Client: “Is it okay to have a glass of wine with dinner?”
Coach: “Totally fair question, and I’m glad you asked. Based on more recent research, we don’t see a health benefit from alcohol, and even small amounts slightly increase some cancer risks.”
Client: “So… should I never have it?”
Coach: “Not necessarily. If you enjoy wine and it’s part of social connection for you, an occasional glass is a fairly small risk. The research suggests keeping it under 4 drinks per week, and less is better.”
Client: “Okay. I can work with that.”
Coach: “Great. My job is to make sure you have accurate information, and then we decide what fits your life.”
For clients who drink more heavily:
- This is a medical and sometimes psychological issue beyond coaching scope
- If someone reports drinking daily or in larger quantities, this warrants referral
- Focus on harm reduction rather than judgment
Practical guidance for those who choose to drink:
- 0-2 drinks/week: Minimal risk
- 3-4 drinks/week: Small but real increase in risk. The upper limit for "tolerable"
- 7+ drinks/week: Clearly elevated risk; recommend reduction
- Daily drinking or binge patterns: Referral territory
If a client decides to keep alcohol in their life, that doesn’t mean they “failed.” It just means you’re both working with real life and real tradeoffs. That’s coaching.
Sex Differences and Context¶
The evidence shows some important variations that can help you personalize the conversation. It’s also why one-size-fits-all advice tends to fall apart.
Women face higher cancer risk from alcohol: Breast cancer risk increases even at low intake levels. One drink daily may increase breast cancer risk by 5-10 percent.
Binge drinking is worse than spread consumption: Four drinks on Saturday is worse than one drink on four separate days, even though the total is the same.
Age matters: The relative risks of alcohol may shift with age. In younger people, alcohol contributes to accidents and risky behavior. In older adults, fall risk and medication interactions become concerns.
What Not to Say¶
Here are common coaching mistakes to watch for (and avoid):
- Don't moralize: "You really shouldn't drink at all" rarely helps and can damage the coaching relationship.
- Don't dismiss concerns: If a client asks about alcohol, they're probably already thinking about it. Take the question seriously.
- Don't oversimplify: "A little is fine" or "any amount is poison" are both inaccurate. Present the gray area clearly.
- Don't push beyond scope: If someone has alcohol dependence or is using alcohol to cope with emotional issues, this needs medical/psychological support, not coaching.
Coaching in Practice: When a client reports drinking more than the tolerable threshold¶
What not to do (examples):
- “Wow, that’s way too much. You need to stop.”
- “Just switch to ‘healthier’ alcohol.”
A supportive, scope-aware dialogue:
Client: “If I’m honest, I’m probably at 10 to 15 drinks most weeks.”
Coach: “Thanks for trusting me with that. No judgment here.”
Coach: “The research is pretty clear that around 10 to 15 drinks per week, health risks start adding up significantly. Would it be helpful to talk about what role alcohol plays in your life, and whether there are any changes you’d actually want to make?”
Client: “Yeah. It helps me unwind, but I don’t love how it’s been going.”
Coach: “That makes a lot of sense. We can start with harm reduction and small steps. And if this feels bigger than a nutrition habit, I can also help connect you with someone who specializes in this area.”
Hydration and Beneficial Beverages¶
Hydration gets overlooked a lot in nutrition conversations, but it affects everything from cognitive function to physical performance to kidney health. It’s not glamorous, but it matters.
Hydration Targets¶
The general guideline: 0.5 to 1 ounce of water per pound of body weight daily. For a 160-pound person, that's 80-160 ounces (roughly 2.5-5 liters). The range depends on activity level, climate, and individual variation.
Practical markers of adequate hydration:
- Urine is pale yellow (not dark, not completely clear)
- No persistent thirst
- Normal energy and cognitive function
When to adjust upward:
- During exercise (especially in heat)
- In hot or dry climates
- When consuming caffeine or alcohol (both have mild diuretic effects)
Most clients underestimate their fluid intake. A simple place to start is tracking water consumption for three days to establish a baseline, then adjusting toward the target range from there. That small bit of data often brings big clarity.
Green Tea: A Special Case¶
The protocol specifically recommends 1 cup of green tea daily. Why single out one beverage?
The evidence:
- Green tea contains catechins (especially EGCG) with antioxidant and anti-inflammatory properties
- Observational studies associate regular green tea consumption with reduced cardiovascular and all-cause mortality
- Meta-analyses suggest 3-5 cups daily shows the strongest associations, but even 1 cup may provide benefit
The practical approach:
- One cup daily is a reasonable target for clients who enjoy tea
- This isn't essential. Clients who dislike tea shouldn't force it
- Green tea contains caffeine (30-50mg per cup), so timing matters for sleep-sensitive individuals
For clients looking to replace less healthy beverages (soda, sweetened coffee drinks), green tea is an excellent swap.
[CHONK: Supplements: Scope-Appropriate Guidance]
Supplements: Staying Within Scope¶
Supplements are where coaches most often overstep their scope, so clear boundaries matter (review Chapter 1.5 if you want a refresher). Clients are often genuinely unsure what to trust here, and it’s normal for them to ask you for a clear answer.
Coaches CAN:
- Educate clients about what supplements are, and how regulation works (and doesn’t)
- Share general evidence about supplement categories, including likely benefits and limitations
- Help clients implement supplement recommendations from their healthcare provider safely and consistently
- Suggest that clients discuss specific supplements with their doctor or dietitian before starting
Coaches CANNOT:
- Recommend specific supplements, brands, or dosages for an individual client
- Diagnose nutrient deficiencies (that requires clinical testing and interpretation)
- Suggest supplements to treat health conditions, symptoms, or lab values
- Sell supplements to clients (a major conflict of interest and scope violation)
The "From Diet First" Principle¶
The protocol emphasizes that supplements are meant to supplement, not replace, a good diet. For most people, a Mediterranean-style eating pattern provides adequate nutrients without supplementation.
Nutrition-Related Supplements Worth Knowing About¶
Omega-3s (EPA/DHA): If clients don't eat fatty fish 2-3 times weekly, omega-3 supplementation (2-3g combined EPA/DHA daily) may fill the gap. Evidence supports cardiovascular and anti-inflammatory benefits.
Vitamin D: Many people are deficient, especially those living at northern latitudes, with dark skin, or who spend little time outdoors. The protocol targets 40-60 ng/mL blood levels, so testing is recommended; common supplementation is 2,000-5,000 IU daily depending on starting levels.
Fiber supplements (psyllium): If dietary fiber intake is insufficient despite efforts, psyllium can help reach targets. It's food-derived and low-risk.
Teaching Clients About Supplement Quality¶
Since you can't recommend specific brands, teach clients what to look for. (This is actually simpler than it sounds.)
Third-party testing certifications:
- USP (United States Pharmacopeia): Tests for identity, strength, purity, and dissolution so the product matches the label
- NSF International: Certifies that products meet label claims and are screened for common contaminants
- ConsumerLab: Runs independent testing and publishes results that clients can look up and review
- Informed Sport/Informed Choice: Tests for banned substances, which is especially relevant for athletes and anyone subject to drug testing
Red flags:
- Products making dramatic health claims ("cures," "reverses aging"), especially when evidence is vague
- Products that are dramatically cheaper than competitors, which can signal lower-quality sourcing
- Products without any third-party verification, seal, or testing information
- Products sold through multi-level marketing, where incentives can distort recommendations
What NOT to do (out of scope):
- Client: “Which brand should I buy, and what dose should I take?”
- Coach: “Buy Brand X and take 3 grams a day.”
A scope-appropriate conversation:
- Client: “Which brand should I buy?”
- Coach: “I can’t recommend specific brands, but I can tell you what to look for. Check the label for third-party testing seals like USP or NSF.”
- Client: “What do those seals actually mean?”
- Coach: “They help verify that what’s on the label is actually in the bottle and that it’s been screened for contaminants. If you’re considering a specific product, it’s a good one to run by your doctor or dietitian.”
[CHONK: Deep Health Integration]
Deep Health Integration¶
Nutrition affects every dimension of Deep Health, not just the physical. Here’s how:
Physical: This one’s pretty obvious: nutrition directly affects metabolic health, body composition, energy levels, and disease risk, which is why it's the primary focus of this chapter.
Emotional: How someone eats affects how they feel about eating, and restrictive diets, food guilt, and constant monitoring can damage emotional health even while "improving" nutrition. As a coach, you’re helping clients build a healthy, enjoyable relationship with food, not anxiety.
What NOT to do:
Coach: "You need to be stricter, so track everything and cut out your favorite foods."
Client: "Honestly, that makes me dread eating."
A better approach:
Client: "I feel guilty every time I eat carbs."
Coach: "That sounds exhausting. Could we focus on one small change this week that supports your goals without making meals feel stressful?"
Social: Food is fundamentally social, and shared meals connect us to family, friends, and culture. Overly rigid nutrition rules can isolate people from social eating, so help clients find approaches that support health while preserving connection.
Environmental: Where food comes from matters to some clients, and concerns like sustainable sourcing, reducing food waste, and supporting local food systems are valid. Meet clients where they are on these issues.
Mental: The MIND diet evidence reminds us that nutrition affects brain function, and blood sugar stability can shape focus and mood. Omega-3s also support neurological health.
Existential: How does someone want to eat for the rest of their life? Nutrition for longevity should align with their values and vision, not just hit macronutrient targets.
[CHONK: Coaching in Practice: A Sample Day]
Coaching in Practice: Putting It Together¶
Case Study: Marcus, 47¶
Background: Marcus is a busy marketing executive who wants to “eat for longevity” after his father’s recent heart attack. Right now, he usually skips breakfast, grabs lunch from nearby restaurants, and eats a large dinner with 2-3 glasses of wine most nights. He’s interested in making changes, and he’s also overwhelmed by all the information (which is totally understandable).
Assessment findings:
- Protein intake: ~70g daily (mostly at dinner)
- Fiber intake: ~12g daily
- Vegetable servings: 1-2 daily
- Alcohol: 15-20 drinks/week
- UPF consumption: Moderate (packaged snacks, some processed meats)
Priority setting: Where do we start?
Instead of trying to fix everything at once (which usually backfires), we can prioritize based on risk, readiness, and what will move the needle fastest.
- Alcohol (highest immediate risk, and the client is receptive to discussing it given his father’s heart attack)
- Protein distribution (adding breakfast protein so it’s not all piled into dinner)
- Vegetable addition (increase without major lifestyle changes)
- UPF reduction (gradual, focused on highest-impact swaps)
A Sample Day (Illustrative, Not Prescriptive)¶
This example shows Mediterranean/MIND principles, adequate protein distribution, and fiber targets. Adapt to your clients' preferences, cultural background, and food access.
If the numbers and food-by-food detail feel like a lot, that’s okay. This isn’t a “perfect day” your client has to copy; it’s just one concrete way to show how the principles can fit together in real life.
Breakfast (~500 calories, ~35g protein, ~8g fiber)
- Greek yogurt (1.5 cups) with walnuts, blueberries, and ground flaxseed
- Coffee with splash of milk
Lunch (~600 calories, ~35g protein, ~12g fiber)
- Large mixed salad with chickpeas, grilled chicken, olive oil/lemon dressing
- Whole grain bread
- Apple
Afternoon snack (~200 calories, ~10g protein, ~5g fiber)
- Hummus with raw vegetables (carrots, cucumbers, bell peppers)
Dinner (~700 calories, ~40g protein, ~15g fiber)
- Grilled salmon with olive oil and herbs
- Roasted vegetables (broccoli, sweet potato, onions)
- Side salad with mixed greens
- Quinoa or whole grain
- Glass of wine (optional, 1 night per week instead of nightly)
Daily totals (approximate):
- Protein: ~120g (distributed ~35/35/10/40)
- Fiber: ~40g
- Vegetables: 8+ servings
- Omega-3s: High (salmon, walnuts, flaxseed)
- Olive oil: Primary fat
- Alcohol: Reduced from 3/night to occasional
Disclaimer: This is an illustrative example showing how the principles come together, not a prescription. Individual needs vary based on body size, activity level, health conditions, and preferences. Clients with specific medical conditions should work with a registered dietitian.
Phased Implementation¶
A phased plan can look like a checklist on paper, but what you’re really doing is building momentum and confidence over time.
Month 1: Foundation
- Add protein to breakfast (primary focus)
- Reduce alcohol to 4 drinks/week maximum
- One coaching conversation about why these matter
Month 2: Building
- Add vegetables to two meals daily
- Introduce meal prep strategies
- Continue alcohol reduction if needed
Month 3: Refining
- Work on fiber diversity
- Address UPF swaps
- Fine-tune based on what's working
If a client doesn’t hit every step perfectly, that’s normal, and you can still look for a clear direction and trend over time rather than flawless execution.
Sample Coaching Conversation¶
Here’s one way a conversation about nutrition for longevity might flow.
Coach: “Marcus, you mentioned wanting to eat for longevity after your dad’s heart attack. Before we get into specifics, what does eating well look like to you right now, and what’s already working?”
Marcus: “I don’t know, honestly. I feel like I should be doing more. I’ve read about all these diets—keto, Mediterranean, intermittent fasting—and I don’t know where to start.”
Coach: “Feeling overwhelmed makes sense. There’s a lot of confident advice out there, and much of it conflicts. What I can tell you is that the research consistently points to a few things that matter most: adequate protein to maintain muscle as you age, lots of vegetables and fiber, mostly whole foods rather than packaged stuff, and being honest about alcohol. Does that feel more manageable than picking one specific diet?”
Marcus: “Yeah, that’s more doable. But where do I start?”
Coach: “Let’s pick one thing for the next couple of weeks so you can get a win. Looking at your typical day, you skip breakfast and then load up at dinner, so a high-impact change would be adding protein to your morning. What feels realistic? Could you do eggs a few days a week, or grab some Greek yogurt?”
Marcus: “I could probably do eggs. I’m just not hungry in the morning.”
Coach: “That’s common when you’ve trained your body to skip breakfast, so start small so this doesn’t feel like a battle. Even two eggs is a good start, about 12-14 grams of protein, and once that becomes routine, we can build up. Does that work as our focus for the next two weeks?”
Marcus: “Yeah, I can do two eggs. Let’s try that.”
Coach: “Perfect. We’ll make a simple plan for that, and we’ll leave everything else alone for now.”
Common Pitfalls to Avoid¶
As you coach nutrition for longevity, a few predictable traps tend to show up:
The perfectionism trap: Clients who try to change everything at once typically burn out, so start with one or two changes and build.
The optimization obsession: Some clients get so focused on optimizing that they miss the basics. If someone’s asking about meal timing while eating fast food daily, redirect to fundamentals.
The fear-based approach: Presenting nutrition as avoiding “bad” foods creates anxiety. Lead with addition (what to include), not just what to avoid.
The scope creep: It’s tempting to give specific supplement recommendations or interpret lab results when clients ask. Stay within scope and refer appropriately.
[CHONK: Study Guide Questions]
Study Guide Questions¶
These questions help you review the chapter and prepare for the exam. While they're optional, we recommend doing them. If you don’t know every answer right away, that’s normal. Use these to guide what you review.
-
How do nutrient-sensing pathways (mTOR, AMPK) connect nutrition to aging biology, and how does this inform the recommendation to avoid chronic caloric excess?
-
What are the key components of the Mediterranean dietary pattern, and what does the evidence show about its effects on mortality and cardiovascular outcomes?
-
Why do older adults need more protein than the standard RDA, what are the per-meal targets, and why does distribution matter?
-
What is the current evidence regarding alcohol and health? How would you explain this to a client who believes moderate drinking is protective?
-
How would you help a client reduce ultra-processed foods without creating food fear or an all-or-nothing approach?
-
What CAN and CANNOT coaches do regarding supplement recommendations? How would you handle a client asking you what supplements to take?
Self-reflection questions:
-
Do a quick protein audit of your own typical day: How much protein do you get at breakfast, lunch, and dinner, and where could you improve protein distribution?
-
How much of your diet comes from ultra-processed foods, and what's one swap you could make this week to shift toward more whole foods?
Optional Articles¶
If you'd like to explore further, these optional articles cover a few key topics from this chapter. Choose one or two that match what you’re most curious about right now.
- How Food Affects Aging Biology: A clear walk-through of the mTOR, AMPK, and sirtuin pathways, and how they connect food intake to aging biology.
- Protein Requirements Research: A closer look at the research behind protein targets, including what changes with age and why per-meal dosing matters.
- Microbiome Science: An explanation of the gut-longevity connection, including what we know, what we don’t, and what’s practical.
- Supplement Evidence Review: A review of the evidence for common longevity supplements, including omega-3s and vitamin D.
References¶
-
Ahmad S, Moorthy MV, Lee I, Ridker PM, Manson JE, Buring JE, et al. Mediterranean Diet Adherence and Risk of All-Cause Mortality in Women. JAMA Network Open. 2024;7(5):e2414322. doi:10.1001/jamanetworkopen.2024.14322
-
Unknown. Mediterranean diet lowers all-cause and cardiovascular mortality for patients with metabolic syndrome. Diabetology & Metabolic Syndrome. 2023. Available at: https://dmsjournal.biomedcentral.com/articles/10.1186/s13098-023-01052-7
-
Adherence to the Mediterranean Diet in Relation to All-Cause Mortality: A Systematic Review and Dose-Response Meta-Analysis. Advances in Nutrition. 2019. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6855973/
-
Ros E, Martínez-González MA, Estruch R, Salas-Salvadó J, Fitó M, Martínez JA, et al. Mediterranean Diet and Cardiovascular Health: Teachings of the PREDIMED Study. Advances in Nutrition. 2014;5(3):330S-336S. doi:10.3945/an.113.005389
-
Mediterranean Diet for Primary Prevention of Cardiovascular Disease. New England Journal of Medicine. 2014;370(14):1368-1368. doi:10.1056/nejmx140016
-
Unknown. Molecular Mechanisms of Healthy Aging: CR, Fasting, Mediterranean and Ketogenic Diets. Nutrients. 2024. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC11397047/
-
Wang VH, GU Y, Gelman A, Divers J, Zhang D. Abstract P2100: Longitudinal association between MIND diet adherence, inflammatory mechanism, and cognitive health. Circulation. 2025;151(Suppl_1). doi:10.1161/cir.151.suppl_1.p2100
-
MIND diet and the risk of dementia: a population-based study. Alzheimer's Research & Therapy. 2022. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC8756695/
-
Agarwal P, Agrawal S, Wagner M, Cherian LJ, Aggarwal NT, James BD, et al. MIND Diet and Hippocampal Sclerosis Among Community-Based Older Adults. JAMA Network Open. 2025;8(8):e2526089. doi:10.1001/jamanetworkopen.2025.26089
-
Lee E, Kim I, Lim S. Physical activity and protein-intake strategies to prevent sarcopenia in older people. International Health. 2025;17(4):423-430. doi:10.1093/inthealth/ihae064
-
N/A. Dietary protein requirements of older adults with sarcopenia. Frontiers in Nutrition. 2025. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC11906324
-
Coelho-Júnior HJ, Calvani R, Tosato M, Landi F, Picca A, Marzetti E. Protein intake and physical function in older adults: A systematic review and meta-analysis. Ageing Research Reviews. 2022;81:101731. doi:10.1016/j.arr.2022.101731
-
Mamerow MM, Mettler JA, English KL, Casperson SL, Arentson-Lantz E, Sheffield-Moore M, et al. Dietary Protein Distribution Positively Influences 24-h Muscle Protein Synthesis in Healthy Adults. The Journal of Nutrition. 2014;144(6):876-880. doi:10.3945/jn.113.185280
-
Taneri PE, Wehrli F, Roa-Díaz ZM, Itodo OA, Salvador D, Raeisi-Dehkordi H, et al. Association Between Ultra-Processed Food Intake and All-Cause Mortality: A Systematic Review and Meta-Analysis. American Journal of Epidemiology. 2022;191(7):1323-1335. doi:10.1093/aje/kwac039
-
Taneri PE, Wehrli F, Roa-Díaz ZM, Itodo OA, Salvador D, Raeisi-Dehkordi H, et al. Association Between Ultra-Processed Food Intake and All-Cause Mortality: A Systematic Review and Meta-Analysis. American Journal of Epidemiology. 2022;191(7):1323-1335. doi:10.1093/aje/kwac039
-
Unknown. Ultra-processed food exposure and adverse health outcomes: umbrella review. BMJ. 2024. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10899807/
-
Lv J, Wei Y, Sun J, Shi Y, Liu F, Sun M, et al. Ultra-processed food consumption and metabolic disease risk: an umbrella review of systematic reviews with meta-analyses of observational studies. Frontiers in Nutrition. 2024;11. doi:10.3389/fnut.2024.1306310
-
Liliani L, Fatmawati F. Association Between Daily Alcohol Intake and Risk of All-Cause Mortality. The International Journal of Medical Science and Health Research. 2024;2(5):35-51. doi:10.70070/gx10jv51
-
Unknown. The relationship between alcohol consumption and health: J-shaped or less is more? BMC Medicine. 2023. Available at: https://bmcmedicine.biomedcentral.com/articles/10.1186/s12916-023-02911-w
-
World Health Organization. No level of alcohol consumption is safe for our health. WHO Europe. 2023. Available at: https://www.who.int/europe/news-room/04-01-2023-no-level-of-alcohol-consumption-is-safe-for-our-health
-
NASEM. Review of Evidence on Alcohol and Health. 2025. Available at: https://www.ncbi.nlm.nih.gov/books/NBK614690/
-
Green CL, Lamming DW, Fontana L. Molecular mechanisms of dietary restriction promoting health and longevity. Nature Reviews Molecular Cell Biology. 2021;23(1):56-73. doi:10.1038/s41580-021-00411-4