Unit 3: Advanced Topics & Disease Prevention¶
Chapter 3.21: Hormone Health for Men¶
[CHONK: 1-minute summary]
What you'll learn in this chapter:
- What actually happens to testosterone as men age, and what doesn't
- Evidence-based lifestyle strategies that support healthy testosterone levels
- What coaches need to know about testosterone replacement therapy (TRT), including fertility considerations
- How to navigate the noise of TRT marketing, "bro science," and supplement hype
- Scope-safe ways to support male clients with hormone-related concerns
The big idea: Testosterone matters for men's health, but the conversation around it has become distorted by aggressive marketing and oversimplified solutions. As a coach, you can be an island of sanity in this noisy space. Your role is to support lifestyle strategies that genuinely influence testosterone (sleep, body composition, stress management, and exercise) while recognizing that testosterone replacement therapy is a medical decision that belongs between a man and his physician. This chapter gives you the knowledge to educate clients accurately, support them effectively, and know exactly when to refer.
Critical scope note: Coaches do not diagnose low testosterone, interpret lab results, or recommend for or against TRT. Instead, we educate, support lifestyle changes, and refer to appropriate medical providers when needed. This chapter is purely educational and equips you to be helpful without crossing into medicine.
Here’s what that can look like in a real coaching conversation, starting with what not to do.
What not to do:
- Coach: “Your testosterone is low, so you should start TRT.”
A scope-safe approach:
- Client: “Do you think I need TRT?”
- Coach: “I can’t diagnose low testosterone or interpret labs, but I can help you work on the lifestyle factors that affect testosterone and help you bring good questions to your physician.”
If hormone talk feels a bit intimidating right now, that's understandable. You don't need to be an endocrinologist to use this chapter well; you'll just need a solid grasp of the big ideas and where your role begins and ends. (We'll walk through that together.)
| For DIY Learners |
|---|
| Applying this to yourself: If you're a man reading this, you've probably encountered testosterone marketing. "Low T" is framed as an epidemic, and TRT is positioned as the obvious solution. But here's what the marketing doesn't tell you: lifestyle factors (sleep, body composition, stress, exercise) have a genuine impact on testosterone levels, and addressing these first is what evidence-based medicine recommends. If you're experiencing symptoms that concern you, by all means talk to your doctor. In the meantime, take an honest look at the foundations, like sleep, body composition, strength training, and chronic stress. Those basics often matter more than people expect. |
[CHONK: Testosterone and Aging: The Reality]
Testosterone and Aging: What Actually Happens¶
Testosterone is the primary male sex hormone. Women have it too, just in smaller amounts, and in men it affects a whole lot more than just libido. No wonder this topic gets so much attention.
In men, it helps regulate:
- Body composition, including muscle mass, strength, bone density, and fat distribution
- Reproductive function, including sex drive, erectile function, and sperm production
- Mood, energy, and red blood cell production
So yes, it’s a big deal, and yes, testosterone levels do decline with age; that part is true. Where things get messy is when marketing tries to turn a gradual, variable biological process into a simple problem with a one-size-fits-all fix.
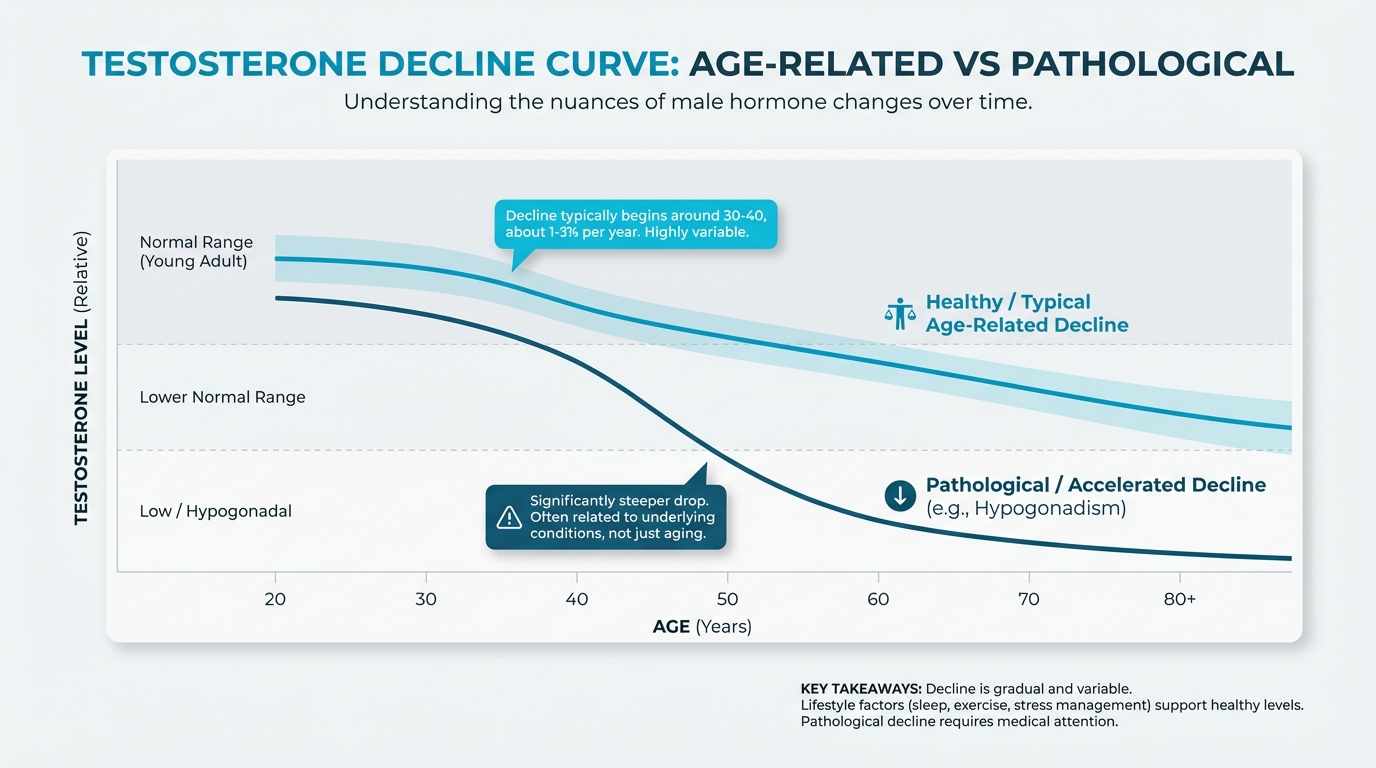
Figure: Age-related decline vs pathological
The Numbers on Decline¶
Here’s what the research shows.
Testosterone typically begins declining around ages 30-40, with estimates ranging from about 1-3 percent per year. A 2024 review in Frontiers in Aging estimated approximately 2.8 percent annual decline in aging men.
The big idea is that decline is gradual and highly variable. Some men maintain healthy testosterone levels well into their 70s and 80s, while others see significant drops earlier. By their 60s, only about 20 percent of men maintain total testosterone in the young-adult normal range. By their 80s, roughly half do.
You don’t need to memorize the exact percentages. The takeaway is that changes are usually slow and highly individual, which also means there’s a wide range of “normal.”
This also isn’t menopause. Women experience an abrupt, universal loss of ovarian function at menopause, whereas men experience a slow, variable decline that’s more like a dimmer switch than an off button. That’s why “andropause” or “male menopause” are misleading terms. The biology is fundamentally different.
What "Low Testosterone" Actually Means¶
Here’s the coaching-relevant takeaway: low testosterone is a medical diagnosis, not something you or your client can determine from symptoms alone.
According to the Endocrine Society and American Urological Association guidelines, diagnosing hypogonadism (the medical term for abnormally low testosterone production) requires:
- Symptoms consistent with androgen deficiency, which we’ll cover below, and that persist over time
- Unequivocally low morning testosterone, measured in the morning and confirmed on at least two separate occasions
- Reliable lab testing, using validated assays and standardized reference ranges
The commonly used threshold is total testosterone below 300 ng/dL (about 10.4 nmol/L), though there's variation across guidelines. The harmonized lower limit for young adult men is around 264 ng/dL.
If you’re not used to thinking in lab cutoffs, don’t worry. You don’t need to recite these numbers to clients; just remember that diagnosis requires both symptoms and properly timed, repeated testing.
Why morning testing matters: Testosterone follows a circadian rhythm, so levels are highest in the morning and decline throughout the day. Testing later in the day can give falsely low results.
Total T vs. Free T vs. SHBG¶
Clients will often mention these terms, so here’s the plain-English version.
Total testosterone is everything in the blood, including testosterone that’s bound to proteins and testosterone that’s “free.”
Free testosterone is the portion that’s not bound to proteins, so it’s available to act on tissues. This represents only about 2-3 percent of total testosterone.
Sex hormone-binding globulin (SHBG) is a protein that binds testosterone and makes it unavailable. As men age, SHBG typically increases, which means that even if total testosterone stays the same, less of it is available to do its job.
If these acronyms feel like a lot, you don’t have to become a lab specialist to coach effectively.
This is why some men with “normal” total testosterone still experience symptoms: their free testosterone may be low because SHBG is high. It’s also why some guidelines recommend checking free testosterone when total testosterone is borderline (200-400 ng/dL).
What this means for your client: If a client brings up these terms, you can explain what they mean educationally. But interpreting whether their specific numbers are “good” or “bad” is for their physician. A scope-safe response sounds like: "That's a great question for your doctor. They can interpret what your specific numbers mean for you."
Symptoms of Low Testosterone¶
Men with genuinely low testosterone may experience:
- Reduced sex drive and erectile dysfunction
- Fatigue, low energy, and difficulty concentrating
- Decreased muscle mass and strength, along with increased body fat (especially around the midsection)
- Mood changes (depression, irritability), decreased bone density, and sometimes hot flashes
The catch: Every single one of these symptoms can be caused by something other than low testosterone, including poor sleep, stress, depression, obesity, medication side effects, or simply aging. That’s why symptoms alone don’t equal a diagnosis; it requires lab confirmation.
As a coach, you’re not expected to untangle all of those possible causes. That’s your client’s medical team’s job, and it’s okay to stay in your lane here.
Why TRT Culture Oversimplifies¶
Your clients are navigating a pretty noisy environment, so it helps to name what’s happening out loud.
Testosterone prescriptions increased 10-fold in the United States and 40-fold in Canada over a single decade, without any new approvals for age-related use. That’s not driven by an epidemic of genuine hypogonadism. It’s driven by marketing.
Some clinics have lowered their thresholds for “low testosterone,” diagnosing men who would be considered normal by major medical guidelines. Some promise benefits that the evidence doesn’t support, and some minimize risks, particularly fertility risks.
Your job isn’t to be anti-TRT; testosterone replacement therapy is a legitimate medical treatment for men with genuine hypogonadism. Your job is to help clients separate evidence from hype, understand what lifestyle can and cannot do, make sure they’re having these conversations with qualified medical providers, and ensure they’re not making decisions based on podcast claims or clinic marketing.
Coaching in practice: When a client says "I think my testosterone is low"¶
The scenario: Your client says, "I think my testosterone is low."
What NOT to do (out of scope): Jump in with, "Yeah, that sounds low. You should get your testosterone tested and probably go on TRT."
Why it doesn't work: That puts you in the role of diagnostician and prescriber, which is outside your scope.
What TO do instead: Stay curious, ask about context, and keep the focus on scope-safe next steps.
Sample dialogue:
Client: "I think my testosterone is low."
Coach: "I hear you. What’s making you think that, and are there specific symptoms you’ve noticed?"
Client: "I'm tired all the time and my sex drive is way down."
Coach: "Those are definitely things worth paying attention to, and low testosterone can be one cause, but sleep, stress, medications, and body composition can also play a role. Low T has to be confirmed with blood tests, ideally morning tests on two separate occasions."
Coach (scope-safe next step): "If this is worrying you, I’d suggest talking with your doctor or a urologist so they can do proper testing and figure out what’s actually going on. In the meantime, we can work on lifestyle factors that support healthy testosterone levels, like sleep, strength training, stress management, and maintaining a healthy body composition."
Avoid saying: "Your testosterone is probably low," "You should get your levels checked," or "Your numbers sound low to me." You’re not qualified to make these assessments.
[CHONK: Supporting Healthy Testosterone Naturally (FIRST)]
Supporting Healthy Testosterone Through Lifestyle¶
Before we get into TRT, which is a medical intervention, it helps to start with what we can actually influence day to day, because this is your home turf as a coach.
Here’s the honest truth: lifestyle strategies can meaningfully influence testosterone levels, but they’re not magic. They tend to work best for men whose testosterone is being pushed down by modifiable factors like excess body fat, poor sleep, or chronic stress. At the same time, they won’t turn a man with genuine hypogonadism into a high-testosterone individual. (Being clear about that up front is part of good coaching, and it helps clients feel supported rather than sold to.)
With that in mind, here’s what the evidence says for each strategy.
Body Composition: The Biggest Lever¶
If there’s one lifestyle factor with the strongest evidence for influencing testosterone, it’s body composition, specifically reducing excess body fat.
The research shows:
- A Mendelian randomization study (which provides causal evidence, not just correlation) found that each standard deviation increase in fat mass was associated with a 0.24 standard deviation decrease in total testosterone.
- Clinical reviews show that weight loss of 5-15 percent typically increases testosterone by 10-30 percent in men who are overweight or obese.
Why does fat matter? Adipose tissue (body fat) contains an enzyme called aromatase that converts testosterone to estrogen, so more fat = more conversion = less testosterone available. Fat tissue also produces inflammatory compounds that can suppress testosterone production.
Visceral fat (the fat around internal organs, which shows up as a bigger waistline) may be particularly problematic, though some imaging studies find that total fat mass matters regardless of location.
What this means for your client: For overweight men concerned about testosterone, weight loss through a sustainable calorie deficit plus exercise is the most evidence-based intervention you can support. The same habits that support weight loss (strength training, adequate protein, better sleep, stress management) also support testosterone through other mechanisms, so you're not chasing a single "hormone hack."
Sleep: Protecting the Foundation¶
Sleep and testosterone are tightly linked, but the relationship is a bit more complex than it might sound. (You don’t need to memorize every detail to coach this well.)
What the research shows:
- Total sleep deprivation (24+ hours) substantially suppresses testosterone. Studies show large reductions (effect size around -0.67).
- Partial sleep restriction (like getting 5-6 hours instead of 7-8) shows less consistent effects in short-term studies. The pooled effect was not statistically significant in one meta-analysis.
- But population data from NHANES (8,748 adults) found that habitual sleep of 6 hours or less was associated with abnormal testosterone levels in men.
If keeping track of those details feels tricky, you’re not alone. The main idea is that chronically short, poor-quality sleep is much more concerning than the occasional late night. (And most clients don’t need perfection here.)
The takeaway is simple: chronic short sleep likely matters more than occasional short nights, and the sleep basics that improve quality (consistent sleep-wake times, a dark room, managing stress) are all things you can absolutely coach.
How to coach this: If a client is consistently getting under 6-7 hours and is concerned about testosterone, sleep improvement is a high-value target because you’re not just addressing testosterone. You’re also supporting everything else sleep affects, like recovery, mood, body composition, and cognitive function.
Strength Training: Building the Infrastructure¶
One finding that surprises many people is that chronic exercise training, including resistance training, does not consistently increase resting testosterone levels in healthy or older men.
A meta-analysis of 11 randomized controlled trials (421 men) found that exercise training had essentially zero effect on resting total testosterone (effect size = 0.00). Another meta-analysis specifically in men over 60 found resistance training did not significantly change basal testosterone.
If you’re thinking, “Wait, what? Didn’t we all hear that lifting weights boosts testosterone?”, you’re not alone.
The more complete picture is that exercise can produce transient, acute increases in testosterone, especially high-intensity work, and in some populations (like young athletes doing intensive training), sustained increases have been observed. But for the typical client, exercise doesn’t reliably raise baseline testosterone levels.
Does that mean exercise doesn’t matter? Absolutely not. Exercise matters enormously for:
- Building muscle mass (which supports metabolic health and body composition)
- Reducing body fat (which we know does increase testosterone)
- Improving insulin sensitivity
- Enhancing mood and energy
- Reducing all-cause mortality
So yes, exercise is essential, but it’s better to avoid promising clients their testosterone will shoot up just from lifting weights, because the evidence doesn’t support that claim.
How to talk about this with clients: Frame strength training honestly. "Strength training builds muscle, helps with body composition, and supports overall metabolic health, which indirectly supports healthy testosterone. I also want to be honest. Research doesn’t show that lifting weights directly raises resting testosterone levels in most men."
Stress Management: The Cortisol Connection¶
Cortisol (the “stress hormone”) and testosterone have an inverse relationship, which means when cortisol goes up, testosterone tends to go down.
Research on police officers and other high-stress populations shows that acute stress elevates cortisol and suppresses testosterone, and the testosterone-to-cortisol ratio declines under stress.
This makes biological sense: when you’re in survival mode, reproduction isn’t a priority, and chronic stress can keep the body in that suppressed state.
What this means for your client: Stress management isn’t just about feeling better, though that matters too. It may support hormonal health, and the interventions overlap with what you’re already coaching: adequate sleep, regular exercise, time in nature, social connection, and explicit stress-reduction practices like meditation or breathwork. (No one needs to do all of these at once, and that’s okay.)
Nutrition: What the Evidence Actually Shows¶
Diet affects testosterone, but not in the ways many people think.
What the research shows:
-
Very low-fat diets lower testosterone. A meta-analysis found that low-fat diet interventions produced modest but significant reductions in serum testosterone compared with higher-fat diets. Men need adequate dietary fat for hormone production.
-
Very high-protein diets (above 3.4 g/kg/day) lower testosterone. This is an extreme intake: for a 180-pound man, that’s over 275 grams of protein daily. Normal high-protein intakes (1.2-2.0 g/kg) do not show this effect.
-
Mediterranean-style diets may support healthy testosterone. A small randomized trial found that a low-carbohydrate, Mediterranean-style diet increased serum testosterone.
Coaching takeaway: No single food or supplement “balances hormones” (despite what you’ll see on social media). The evidence points to overall dietary patterns: adequate but not excessive protein, sufficient healthy fats, plenty of vegetables, and avoiding extreme restrictions. This is standard good nutrition, and that’s the point: nothing magical required. (No “testosterone superfood” shopping list needed.)
What Lifestyle Can and Cannot Achieve¶
Realistic expectations matter here, because they protect your client from false hope and they protect you from overpromising. (This can be a sensitive conversation, so it helps to lead with empathy.)
Lifestyle strategies CAN:
- Support healthy testosterone in men whose levels are being suppressed by modifiable factors (obesity, poor sleep, chronic stress)
- Improve overall health, energy, and body composition, which matters regardless of testosterone numbers
- Prevent further decline by maintaining healthy habits
Lifestyle strategies CANNOT:
- "Cure" genuine hypogonadism caused by testicular or pituitary disease
- Raise testosterone to supraphysiologic levels
- Substitute for medical treatment in men who truly need it
What this means for your client: Be honest. "Lifestyle changes can make a real difference, especially if there are modifiable factors contributing to your symptoms. But if there’s an underlying medical condition, lifestyle alone may not be enough, and that’s where working with your doctor becomes important." Being upfront about these limits builds trust, and if a client feels discouraged by that, that’s normal.
| For DIY Learners |
|---|
| Applying this to yourself: Before you start researching TRT clinics or "testosterone-boosting" supplements, honestly assess the foundations. Are you sleeping less than 7 hours regularly? Carrying significant abdominal fat? Chronically stressed? Sedentary or doing only cardio without strength training? Eating a very low-fat or extremely high-protein diet? If any of these apply, you have modifiable factors that could be affecting your testosterone, and these are worth addressing first. This isn't about dismissing your symptoms; it’s about optimizing the things that are genuinely in your control before jumping to medical interventions. |
Coaching in practice: Building a lifestyle game plan for testosterone support¶
The scenario: Your client is worried about testosterone and wants to know what to do.
What NOT to do: Jump straight to lab numbers or supplements without understanding what daily life looks like, because that skips over the biggest levers you can actually help with.
What TO do instead: Start with a clear picture of your client’s sleep, movement, stress, and nutrition, then pick one or two big wins.
Sample dialogue (first-session focus):
Coach: "Since you’re worried about testosterone, can I ask a few questions about sleep, movement, stress, and nutrition? Those are the areas we know make the biggest difference."
Client: "Sure."
Coach: "To start, how many hours of sleep do you usually get, and how’s your stress level these days?"
Client: "Honestly, I sleep about 5 hours and I'm stressed most of the time."
Coach: "Thanks for sharing that. Based on what you've told me, it sounds like sleep and late-night snacking are the biggest opportunities right now. How would you feel about focusing on those first, and keeping everything else pretty simple for the moment?"
Practical checklist you can use:
- Get a clear picture of their lifestyle:
- Sleep: How many hours? How consistent? Quality indicators?
- Body composition: What's the waist circumference? Trend over time?
- Exercise: Strength training frequency? Types of movement?
- Stress: Chronic stressors? Recovery practices?
- Nutrition: Overall pattern? Protein adequacy? Fat intake? Alcohol?
- Prioritize based on biggest gaps:
- Overweight client sleeping 5 hours → Sleep and body composition are priorities
- Lean client with high stress → Stress management and sleep
- Set realistic expectations:
"These changes support overall health and may help with the symptoms you’re experiencing. If we make progress on these and you’re still concerned, or if symptoms are significant, that’s when getting proper testing from your doctor makes sense." - Track progress on what matters:
Energy, mood, sleep quality, body composition, and strength; not testosterone numbers (which you can't interpret anyway).
[CHONK: TRT: What Coaches Should Know (Educational)]
Testosterone Replacement Therapy: What Coaches Should Know¶
This section covers testosterone replacement therapy (TRT), not so you can advise on it, but so you can recognize what it is and speak to it at a high level when clients bring it up.
Critical reminder: Everything in this section is educational only, and coaches do not recommend for or against TRT because this is a medical decision between a patient and their physician.
When TRT Is Medically Appropriate¶
According to major medical guidelines (Endocrine Society, American Urological Association), testosterone therapy is indicated for men with:
- Consistent symptoms of androgen deficiency that persist over time
- Unequivocally low testosterone confirmed on at least two separate morning tests
- After appropriate workup to identify and address underlying (and potentially reversible) causes
Treatment is NOT recommended for:
- Asymptomatic men with low testosterone numbers on labs alone
- Men with borderline-low testosterone who haven't had repeat confirmation testing
- Men with reversible causes of low testosterone (like obesity) that should be addressed first, when possible
How TRT Works¶
Testosterone replacement provides exogenous (from outside the body) testosterone to restore levels to the normal range. It comes in several forms:
- Injections (intramuscular or subcutaneous): Most common, often done at home, with levels that can fluctuate between injections.
- Transdermal gels or patches: Applied daily, with more stable levels, but with a risk of transfer to partners/children.
- Pellets: Implanted under the skin every 3-6 months, which can provide consistent levels but requires a procedure.
- Oral formulations: Newer options that avoid the liver issues of older oral testosterone and are less commonly used.
The goal is to achieve testosterone levels in the mid-normal range, not supraphysiologic peaks.
What the Evidence Shows About Benefits¶
Recent high-quality evidence has clarified what TRT can and cannot do:
Sexual function: The TRAVERSE trial (the largest cardiovascular safety trial of TRT) found that testosterone improved sexual activity (about 0.47 more acts per day compared to placebo) and sexual desire. However, erectile function did not significantly improve compared to placebo in this study. Translation: TRT may help with desire and activity, but it's not necessarily a fix for erectile dysfunction.
Energy and vitality: Benefits here are more modest and inconsistent. The Endocrine Society Scientific Statement notes "minimal benefits in vitality/strength" from trials in older men.
Body composition: Some improvement in lean mass and reduction in fat mass, though effects are modest.
Bone density: Improvements observed, particularly relevant for men with osteoporosis.
Mood: Some improvement in mood and depressive symptoms in hypogonadal men.
If it feels hard to keep all of those domains straight, that's OK.
The simple takeaway is that TRT can help with specific symptoms in men who truly have low testosterone, but it isn't a cure-all.
Cardiovascular Safety: The Current Evidence¶
This has been a major question, and the evidence has evolved:
The TRAVERSE trial (published in New England Journal of Medicine, 2023) enrolled about 5,200 men aged 45-80 with low testosterone and existing cardiovascular risk factors or cardiovascular disease. Over about 2 years:
- Primary endpoint (cardiovascular death, nonfatal heart attack, nonfatal stroke): 7.0% in TRT group vs. 7.3% in placebo group, with no significant difference. The trial demonstrated non-inferiority for cardiovascular safety.
Meta-analyses of 26-35 randomized trials consistently show no increase in major cardiovascular events, heart attacks, strokes, or mortality with TRT in hypogonadal men.
However: The TRAVERSE trial did find higher incidences of atrial fibrillation, acute kidney injury, and pulmonary embolism in the testosterone group. These signals warrant monitoring.
Bottom line: For men with genuine hypogonadism who are appropriately monitored, current evidence does not show increased major cardiovascular events. But it's not risk-free, so monitoring matters.
You don't need to weigh in on study details; you just need to know that appropriate medical monitoring is essential.
Bottom line for coaching
What NOT to do:
- Client: "Is TRT safe for my heart?"
- Coach: "Yes, it's totally safe" (or "No, it's dangerous, don't do it").
What TO do instead (sample dialogue):
- Client: "Is TRT safe for my heart?"
- Coach: "That's a great question for your prescriber. What I can tell you is that TRT isn't risk-free, and it should come with regular medical monitoring. If you're open to it, we can also focus our work on the lifestyle basics that support cardiovascular health while your doctor manages the medical side."
Side Effects and Monitoring Requirements¶
TRT requires ongoing medical supervision. Here's what physicians monitor:
Erythrocytosis (elevated red blood cells): This is the most common side effect. Testosterone stimulates red blood cell production, which can thicken the blood and potentially increase clotting risk.
- Guidelines recommend checking hematocrit at baseline, at 3 months, and then at least annually; if it exceeds about 52-54%, dose adjustment or therapeutic phlebotomy (blood removal) may be needed
- One study found that about 40% of therapeutic phlebotomies at a blood center were for men on testosterone therapy
Prostate monitoring: Current evidence does not show increased prostate cancer incidence in men on monitored TRT. However:
- TRT is contraindicated in men with active, untreated prostate cancer
- PSA and digital rectal exam are monitored at baseline, 3 months, and annually
- Rising PSA warrants urology referral

Figure: When to refer to endocrinologist
Other potential side effects:
- Skin and mood effects: acne/oily skin, and sometimes mood changes
- Sleep apnea (can worsen existing sleep apnea)
- Hormone and size changes: breast enlargement (gynecomastia) if testosterone converts to estrogen, and testicular shrinkage (because the body reduces its own production)
Key point: responsible TRT comes with regular lab work and safety checks, not just a prescription.
CRITICAL: Fertility Implications¶
This section matters enormously, and it's often minimized or ignored in TRT discussions. Exogenous testosterone suppresses sperm production.
Here's the mechanism: When you give testosterone from outside the body, the brain senses "there's enough testosterone" and stops sending signals (LH and FSH) to the testicles to produce more. Without that signal, the testicles not only stop making testosterone, they also stop making sperm.
The statistics are striking:
- Intratesticular testosterone (the testosterone inside the testicles, which is required for sperm production) must fall by more than 80% before spermatogenesis declines. Exogenous testosterone causes exactly this.
- Most men develop severe oligozoospermia (very low sperm count) or azoospermia (zero sperm) within 3-6 months of starting TRT.
- Azoospermia rates reach 90% or higher in controlled male contraceptive trials using testosterone.
- Testicular volume typically decreases by 16-30% during TRT.
Can fertility recover after stopping TRT?
In men who used testosterone for contraceptive studies (typically healthy men with normal baseline fertility):
- About 67% recover to fertile sperm counts by 6 months after stopping, about 90-98% recover by 12 months, and nearly 100% recover by 24 months
But: Recovery is slower and often incomplete in men who used TRT long-term (years) or who used anabolic-androgenic steroids at higher doses. In one study of men with prior anabolic steroid use presenting to an infertility clinic, 51% were azoospermic at presentation. Even with treatment (clomiphene + hCG), only 5.6% of initially azoospermic men achieved normal sperm counts at 6 months. For these men, "I'll just come off later and everything will bounce back" isn't always true.
What about preserving fertility while on TRT?
Human chorionic gonadotropin (hCG) mimics the signal (LH) that tells the testicles to produce testosterone. When used alongside TRT, it can maintain intratesticular testosterone and preserve spermatogenesis. Current guidelines recommend gonadotropin therapy (hCG with or without FSH) rather than exogenous testosterone for hypogonadal men who desire future fertility.
What this means for coaching: Any man considering TRT who might want children in the future needs to understand these implications before starting. This isn't optional information. It's essential.
The stakes can be high for clients.
Bottom line for coaching
What NOT to do:
- Client: "My doctor mentioned TRT. We might want kids someday."
- Coach: "You can always come off later. You'll be fine."
What TO do instead (sample dialogue):
- Client: "My doctor mentioned TRT. We might want kids someday."
- Coach: "I'm glad you brought that up. One thing to know is that TRT can significantly suppress sperm production while you're on it. Have you and your doctor talked through the fertility implications and any fertility-preserving options before you make a decision?"
Coaching in practice: Explaining fertility implications to clients considering TRT¶
The scenario: A client is considering TRT and may want children in the future.
What NOT to do: Skip over fertility or say, "You can always come off later and you'll be fine."
Why it doesn't work: That minimizes real risks and goes beyond your scope.
What TO do instead: Ask whether future fertility matters to them, share high-level education, and point them back to their doctor for specifics.
Sample dialogue:
Coach: "You mentioned your clinic suggested TRT. Can I ask: Do you have kids already, or is having (more) children something that might matter to you in the future?"
Client: "We might want another child in a few years, but I'm not sure."
Coach: "Thanks for sharing that. One important piece that sometimes gets glossed over is that testosterone replacement can significantly suppress sperm production, often to very low or even zero levels while you're on it. For many men this is reversible after stopping, but it can take many months, and recovery isn't guaranteed, especially with long-term use."
Coach: "If fertility is on your radar at all, it's really important to talk this through with your doctor before starting. There are medical approaches that can help preserve fertility, but they need to be planned in advance."
Scope reminder: Don't advise them whether to start or stop TRT, interpret whether their fertility risk is high or low, or recommend specific protocols. That's their doctor's role.
[CHONK: The TRT Culture Problem]
Navigating the TRT World: Evidence vs. Marketing¶
Your clients are exposed to a ton of information about testosterone from podcasts, ads, social media influencers, and friends at the gym, and honestly, a lot of it is misleading (or at least oversold).
When you understand the environment they’re swimming in, you can be a credible, steady voice amid the noise. You don’t have to be an endocrinologist to do that; you just have to help clients slow down and think clearly about what they’re hearing, what’s evidence-based, and what’s mostly marketing. (In other words, you’re helping them sort signal from noise.)
Most clients feel the same way when they first start looking into TRT.
TRT Clinics vs. Evidence-Based Medicine¶
Not all TRT is created equal, and there can be a meaningful (and sometimes concerning) difference between how it’s prescribed and monitored across settings. (This is where guidelines really matter.)
Evidence-based TRT (through endocrinologists, urologists, or primary care physicians following guidelines):
- Diagnosis requires confirmed symptoms and confirmed low testosterone on repeat morning tests
- Treatment targets mid-normal testosterone levels, rather than pushing the high end
- Regular monitoring of hematocrit, PSA, and symptoms
- Discussion of fertility implications up front
- Appropriate patient selection based on risk and benefit
Marketing-driven TRT (some, not all, specialty clinics):
- May diagnose based on symptoms alone or a single test
- May use thresholds lower than major guidelines
- May target testosterone levels above the normal range
- May minimize or omit discussion of risks and fertility implications
- May market heavily with promises of life transformation
This isn’t to say all TRT clinics are problematic, because many provide excellent care. The challenge is that standards can vary a lot, and your clients may not know how to tell the difference. (Most people assume “a clinic” automatically means “best practice,” and that’s not always true.)
The "More Is Better" Myth¶
A risky idea floating around fitness culture is: If normal testosterone is good, higher must be better. That belief can lead people toward supraphysiologic dosing, meaning testosterone doses that push levels well above the normal range. (Bigger numbers aren’t automatically better. Not even close.)
Here’s what the evidence shows about supraphysiologic testosterone:
Cardiovascular effects: TRT at physiologic doses appears cardiovascular-neutral, but animal studies show supraphysiologic testosterone induces vascular dysfunction through oxidative stress and inflammation pathways. In humans, TRT-induced polycythemia (elevated red blood cells) is associated with increased risk of major adverse cardiovascular events and venous thromboembolism (odds ratio approximately 1.35).
Neurobehavioral effects: Research on anabolic-androgenic steroid users (who use supraphysiologic doses) shows impaired recognition of negative facial expressions compared to non-users. More concerning, approximately 30% of anabolic-androgenic steroid users develop dependence. (That number tends to surprise people.)
Greater suppression of the HPG axis: Higher doses mean more profound suppression of the body’s natural testosterone production and more complete suppression of sperm production.
The regulatory picture is also clarifying. In 2025, the FDA determined that appropriately indicated TRT does not show increased cardiovascular risk, and removed prior general cardiovascular risk warnings from labels; however, they added warnings about blood pressure increases for certain formulations. The message: physiologic replacement with monitoring is one thing; pushing levels beyond normal is another.
(If this part feels a little scary or heavy, that’s normal. The goal here isn’t to panic, but to help clients make informed, medically sound decisions.)
Red Flags in TRT Marketing¶
Clients do best when they can spot marketing that’s getting ahead of the evidence. Here are some red flags to watch for:
- Promises of dramatic life transformation, even though the evidence points to modest benefits in specific domains, not wholesale change.
- "Every man over 40 should consider it," even though no guideline supports this. TRT is for men with confirmed hypogonadism.
- Dismissal of fertility concerns, including "don't worry about that" or skipping the fertility conversation entirely.
- Targeting "optimal" rather than "normal," since chasing supraphysiologic levels is not evidence-based.
- Downplaying monitoring needs, even though legitimate TRT requires ongoing monitoring.
- Aggressive upselling of supplements, peptides, or other add-ons.
Why this is so emotionally loaded for men¶
Marketing often skips an important piece of context: testosterone is deeply tied to masculine identity for many men. So when symptoms like fatigue, low libido, or declining strength show up, they don’t just feel like “health problems.” They can feel like threats to who someone is. (This is more common than people admit out loud.)
That's why messages like "get your edge back" or "feel like a man again" can land so hard, and it's also why it can be tough, in the moment, to hear that the first step might be better sleep and stress management rather than a prescription.
Approach these conversations with real compassion. The underlying fear (“Am I losing something fundamental about myself?”) is real, even if the marketing solution isn’t always the right answer, so validate the concern first and then help them come back to evidence. (If you’re not sure what to say, you’re not alone. These are tender conversations.)
Being a Steady Voice¶
Your role isn’t to be anti-TRT. Testosterone replacement is a legitimate treatment for men with genuine hypogonadism, and your job is to help clients navigate the decision well by focusing on four things. If they’re feeling pulled in ten directions by what they’ve heard online, this gives you a simple way to bring them back to solid ground. (And you don’t have to memorize this.)
-
Understand what lifestyle can address first. Many symptoms attributed to "low testosterone" improve with sleep, stress management, and body composition changes.
-
Seek proper diagnosis: Symptoms alone aren’t enough, so proper testing (morning, repeated) through appropriate medical providers matters.
-
Ask the right questions. For example: "What's my actual testosterone level?" "Have we confirmed this with a repeat test?" "What are the fertility implications?" and "What's the monitoring schedule?"
-
Distinguish marketing from medicine. The flashier the promise, the more skeptical they should be.
Coaching in practice: When a client brings in TRT clinic marketing¶
The scenario: A client brings in TRT clinic marketing and asks what you think.
What NOT to do: Roll your eyes or say, "That place is a scam, stay away." That can shut down the conversation and put you in the role of adversary instead of ally.
What TO do instead: Validate their concerns, then help them think through good questions to ask.
Sample dialogue:
Client: "I saw this clinic that says they can 'optimize my hormones' and get me back to how I felt at 25. What do you think?"
Coach: "I can see why that caught your attention. A lot of guys are hearing the same messaging right now. Before we decide if it’s a great fit or a bad fit, can I ask what you’re hoping TRT would help with?" (This helps you stay on their side.)
Client: "Mostly energy and motivation. I’m dragging, and my workouts aren’t what they used to be."
Coach: "That makes total sense. Feeling flat is frustrating, and it’s easy to hope there’s one clear answer. Some clinics do great work, and others make bigger promises than the evidence supports, so the best next step is usually to slow down and get specific. Would it be okay if we looked at a few questions you could ask them or your doctor?"
Client: "Yeah, that would help. I don’t even know what to ask."
Coach: "You’re not alone. Here are a few that quickly separate evidence-based care from pure marketing."
Share evaluation questions: Some good questions to ask include:
- "How do you diagnose low testosterone? Is it based on symptoms alone, or will you confirm it with repeat morning lab tests?"
- "What levels are you targeting: mid-normal or higher?"
- "What's your monitoring protocol, and how often will we recheck key markers?"
- "How do you handle fertility considerations?"
Client: "Okay, I can ask those. If they dodge the questions, that’s probably a sign."
Coach: "Exactly. And if you want a second opinion, you could also talk to your primary care doctor, a urologist, or an endocrinologist. They follow established guidelines and can provide a second perspective."
Client: "So you’re not saying ‘never TRT,’ you’re saying ‘do it the right way.’"
Coach: "You’ve got it. And my job is to help you with the lifestyle factors that support your health: sleep, exercise, stress, nutrition. Those things matter regardless of what you decide about TRT, and they’re often the first things worth addressing before jumping to medical interventions."
[CHONK: Coaching Men Through Hormonal Concerns]
Coaching Men Through Hormone-Related Concerns¶
Let's get practical about your coaching role. This section outlines exactly what you can do, what you cannot do, and how to handle common scenarios.
It’s common to feel a little nervous about saying the "wrong" thing with hormones. That's OK. Caring about scope is part of being a professional.
What Coaches CAN Do¶
Educate about testosterone and aging. You can share the information in this chapter about what testosterone does, how it changes with age, and what symptoms may indicate low testosterone. Education helps clients understand their situation and ask better questions of their physicians.
Support lifestyle strategies that influence hormone health. This is your core domain. Sleep, body composition, stress management, exercise, nutrition. These all matter for testosterone and for overall health. You can assess where clients stand, help them prioritize, and support behavior change.
Explain what research shows about TRT (without recommending). "Research shows that TRT can improve sexual desire and activity in men with confirmed low testosterone, but it doesn't necessarily fix erectile dysfunction. It also has side effects that require monitoring, especially effects on blood count and fertility." This is education, not recommendation.
Discuss fertility implications. Sharing what exogenous testosterone does to sperm production is educational and important. Encouraging clients to discuss this with their doctor before starting TRT is appropriate.
Encourage appropriate medical evaluation. If a client has symptoms that concern them, suggesting they discuss it with a doctor is helpful and within scope. "That sounds like something worth getting checked out" is fine. "You should get your testosterone tested" starts to cross the line.
Support clients who are already on TRT (without advising on it). If a client is on TRT, you can support their lifestyle, helping them with nutrition, exercise, sleep, stress management. You can ask how they're feeling, whether they're keeping up with monitoring appointments. What you cannot do is comment on whether their dose is appropriate, whether they should continue, or interpret their lab results.
What Coaches CANNOT Do¶
Some of these might feel obvious. Others less so.
Recommend for or against TRT. "I think you should consider TRT" or "I don't think you need TRT" are both outside scope. The decision is medical.
Interpret testosterone test results. "Your testosterone is low" or "That number is fine" are medical interpretations, even if they seem straightforward.
Suggest specific TRT formulations or doses. "Injections are better than gels" or "You should ask about hCG" crosses into medical territory.
Advise on starting, stopping, or adjusting TRT. "Maybe you should try a lower dose" or "Have you thought about coming off it?" are medical decisions.
Diagnose low testosterone or hypogonadism. Even if a client shows you labs, you cannot diagnose. You can acknowledge symptoms and recommend medical evaluation.
Provide opinions on "ideal" testosterone levels. "600 is where you want to be" is not something you're qualified to say.
Scope-Safe Language Patterns¶
Language matters. Here are patterns that keep you in scope:
INSTEAD OF: "You should get your testosterone tested."
SAY: "If you're experiencing those symptoms, it might be worth bringing up with your doctor."
INSTEAD OF: "That testosterone level is low."
SAY: "I can see why you're concerned. Your doctor can help you understand what your numbers mean and whether treatment is indicated."
INSTEAD OF: "TRT would probably help you."
SAY: "Some men with confirmed low testosterone see benefits from treatment. That's something to explore with your physician if testing shows that's what's going on."
INSTEAD OF: "I don't think you need TRT."
SAY: "There are lifestyle factors that can influence testosterone and energy. Would you like to work on those first and see how you feel? If symptoms persist, you can always revisit testing with your doctor."
INSTEAD OF: "Your TRT dose seems high."
SAY: "How are you feeling on your current regimen? Are you staying on top of your monitoring appointments?"
| For DIY Learners |
|---|
| Applying this to yourself: If you're considering TRT, here are the questions to ask your doctor (not a clinic's marketing team): Is my testosterone actually low on properly-timed, repeated tests? Have we ruled out reversible causes like sleep apnea, obesity, or medication effects? What are the fertility implications? What monitoring will be required? What's the exit strategy if I want to stop? And be honest with yourself: Have you actually optimized the lifestyle factors first (consistently sleeping 7+ hours, managing stress, doing regular strength training, maintaining healthy body composition)? If not, start there. You may be surprised by the results. |
When to Refer: Specific Criteria¶
Referral to appropriate medical providers is part of your role. Here are clear triggers:
Refer when a client:
- Has symptoms suggestive of low testosterone (reduced libido, fatigue, mood changes, decreased muscle/strength, erectile dysfunction) that haven't been medically evaluated
- Asks about TRT or wants to pursue it
- Has lab results they want interpreted
- Shows signs of potential pituitary issues (severe headaches, visual changes, multiple hormone abnormalities)
- Has fertility concerns alongside testosterone concerns
- Is requesting supplement recommendations for testosterone support
- Has symptoms that aren't improving despite lifestyle changes
Where to refer:
- Primary care physician (for initial evaluation and basic testing)
- Urologist (specializes in male reproductive and hormonal health)
- Endocrinologist (for complex hormonal conditions, pituitary issues)
Working with Medical Teams: Triangle of Care¶
Remember the Triangle of Care model from Chapter 1.5: Client, Coach, Physician working together. That's especially important here.
Your role is complementary to medical care, not a replacement for it. For men with confirmed hypogonadism on TRT, you can:
- Support adherence to their treatment plan
- Help with lifestyle factors that complement treatment
- Encourage them to maintain monitoring appointments
- Notice if they're having difficulties they should bring up with their doctor
What you cannot do is make adjustments to the medical side of their care. That line might feel frustrating sometimes, but it's there for good reasons, and crossing it puts both you and your client at risk.
Coaching in practice: Scope-safe responses to common testosterone questions¶
The scenario: Clients ask direct questions about testosterone, TRT, or lab results.
What NOT to do (general pattern): Give direct medical advice, interpret lab results, or reassure/dismiss in ways that a physician should.
What TO do instead: Acknowledge the question, stay in your lane, and use language that points back to their medical team while keeping coaching momentum.
When a client asks, "What testosterone level should I aim for?"
You might say: "That's really a question for your doctor. Guidelines target mid-normal ranges, but what's appropriate for you specifically depends on your symptoms, your health history, and your individual response."
When a client asks, "What supplements boost testosterone?"
You might say: "I'm not able to recommend supplements. That's outside my scope as a coach. What I can tell you is that the evidence for most 'testosterone-boosting' supplements is pretty weak. The lifestyle factors that have the most evidence (sleep, body composition, stress management, strength training) are things we can absolutely work on together."
When a client asks, "Should I start TRT?"
You might say: "That's a medical decision I'm not qualified to make. What I can say is that if you're experiencing symptoms, getting properly evaluated is worthwhile. And regardless of what you decide about TRT, the lifestyle factors we work on matter for your health."
When a client says, "My testosterone came back at 350. Is that low?"
You might say: "I can't interpret lab results for you, but that's definitely a question for your doctor. They can tell you what your number means in context of your symptoms, your age, and whether repeat testing is indicated."
[CHONK: Deep Health Integration]
Testosterone and Deep Health: The Bigger Picture¶
Testosterone doesn't exist in isolation. Like everything we work on in coaching, it's connected to all six dimensions of Deep Health, which means there are lots of useful places to start.
Physical¶
Testosterone influences muscle mass, bone density, fat distribution, energy, and sexual function, but the relationship goes both ways: physical health practices like exercise, sleep, and nutrition also influence testosterone. This is often where your coaching can have the most direct, practical impact. The basics really do matter.
Emotional¶
Testosterone can affect mood, and men with genuinely low testosterone often report depressive symptoms, irritability, and emotional flatness. At the same time, depression, stress, and anxiety can suppress testosterone, which means emotional health work may support hormones, and hormone-related support may help mood too.
For some men, testosterone concerns are tightly tied to feelings about aging, masculinity, and self-worth. Sensitivity matters here. The goal isn't to dismiss these feelings; it's to support the whole person while staying in scope.
Mental/Cognitive¶
Some men with low testosterone report cognitive symptoms like “brain fog,” difficulty concentrating, and memory issues. The evidence connecting testosterone to cognition is complex and not fully settled, but we do know that the lifestyle factors that support testosterone, such as sleep, exercise, and stress management, also support cognitive function through multiple pathways.
Social¶
Testosterone influences libido and sexual function, which can affect intimate relationships, and low energy or mood changes can shape social engagement more broadly. When you’re supporting men with testosterone concerns, keep the relational context in view. Sometimes the distress isn’t just about numbers on a lab report; it’s about how they feel in their relationships and day-to-day life. That distinction matters.
Environmental¶
Endocrine disruptors, which are chemicals that can interfere with hormone function, show up in many consumer products. While the degree to which they affect testosterone in real-world exposures is debated, minimizing exposure to things like BPA, phthalates, and certain pesticides is reasonable. This connects to the environmental health work covered elsewhere in the curriculum.
Existential¶
For many men, concerns about testosterone are really concerns about aging, capability, and identity: “Am I still the man I was?” “Am I declining?” “Will I be able to do the things that matter to me?”
This is existential territory, and your role isn’t to promise that addressing testosterone will solve these concerns. It’s to support clients in living well and maintaining the health, strength, and vitality to pursue what matters to them, regardless of their testosterone numbers. You don’t need perfect words for every fear. Often, listening, reflecting back what you’re hearing, and staying curious goes a long way. If this part feels heavy, that’s normal.
Common Mistakes to Avoid: Coaching Men Through Midlife and Beyond¶
As a coach working with men, especially those concerned about testosterone, aging, or overall vitality, you’ll see some common patterns that can quietly undermine health. Here are mistakes to watch for, along with what you can help clients do instead.
Ignoring cardiovascular exercise. Many men who lift weights neglect their cardiovascular system, sometimes because they think cardio interferes with muscle gains and sometimes because they simply prefer the gym to running or cycling. But cardiovascular health is foundational for longevity, and Zone 2 cardio specifically supports metabolic health, recovery, and even testosterone levels indirectly through better sleep and reduced visceral fat. Help clients understand that strength and cardio aren’t enemies; they’re teammates, and both are essential.
Suppressing emotions. Cultural conditioning leads many men to minimize, avoid, or “power through” emotional distress, but that distress doesn’t disappear. It often shows up as chronic stress, poor sleep, relationship problems, or unhealthy coping behaviors (alcohol, overwork, isolation). As a coach, you can normalize emotional awareness without being a therapist, and sometimes a simple question like “How are you really doing?” is enough to open a door.
Avoiding medical care. Men are less likely than women to see doctors regularly, get recommended screenings, or address health concerns early, and many only seek care when something is seriously wrong. Encourage annual checkups, proactive bloodwork, and addressing symptoms rather than ignoring them. “Tough it out” isn’t a longevity strategy.
Excessive alcohol consumption. Alcohol is a common social lubricant and stress reliever for many men, but it directly suppresses testosterone, impairs sleep quality, contributes to visceral fat accumulation, and increases multiple disease risks. Help clients examine their relationship with alcohol honestly. The protocol suggests 2-4 drinks per week maximum, which is significantly less than many men consume.
Neglecting flexibility and mobility. Many men focus on strength or endurance and ignore mobility work until something hurts, but flexibility and joint health become increasingly important with age. Stiff, immobile men are more likely to get injured, limit their activity options, and lose functional capacity. Building a daily mobility practice (even 10-15 minutes) pays dividends for decades.
Coaching in practice¶
What NOT to do
Client: “My buddy says I just need to raise my testosterone, so should I get on TRT?”
Coach: “You should focus on sleep, Zone 2, mobility, stress, and cutting alcohol. Also get labs and see your doctor.”
A better approach
Client: “My buddy says I just need to raise my testosterone, so should I get on TRT?”
Coach: “I can see why you’d want a clear answer, especially with all the advice out there. Before we talk about TRT, can I ask what’s been feeling most off lately: energy, mood, libido, or training recovery?”
Client: “Mostly energy and recovery.”
Coach: “Got it. A good next step is to cover the basics that tend to move both recovery and hormone health: consistent sleep, some Zone 2 cardio, and strength training that you can recover from. And if symptoms persist, that’s a good cue to bring a clinician in for labs and a medical discussion.”
Understanding these patterns helps you proactively guide male clients away from common pitfalls and toward strategies that support their long-term health and vitality.
[CHONK: Study guide questions]
Study Guide Questions¶
Here are some questions that can help you think through the material and prepare for the chapter exam. They're optional, but we recommend answering at least a few to reinforce what you've learned.
-
What's the difference between "andropause" and menopause, and why does this distinction matter for how you educate clients?
-
A client asks you to look at their testosterone lab results and tell them if they're "low." What do you say, and why?
-
Of the lifestyle factors that influence testosterone, which has the strongest evidence, and what's a realistic expectation for its effect?
-
What does exogenous testosterone do to sperm production, and why is this important information for clients to know before starting TRT?
-
How would you distinguish between evidence-based TRT practice and marketing-driven practice, and what are some "red flags" in TRT marketing?
-
Give an example of scope-safe language for each of these situations:
- A client wants to know if their testosterone is "good" and what that means for their health
- A client asks if they should start TRT and wants your take on the risks and benefits
-
A client asks what supplements boost testosterone, and whether any are worth trying
-
When should you refer a client to a medical provider for testosterone-related concerns? List at least three specific situations.
-
What is polycythemia (erythrocytosis), and why is it monitored in men on TRT?
Self-reflection questions:
-
If you're a man: Before considering any testosterone intervention, how solid are your fundamentals, like sleep, stress management, exercise, and body composition? These matter more than any supplement.
-
How has marketing shaped your beliefs about testosterone and aging, and where might you have absorbed messages that aren't supported by evidence?
Works cited¶
References¶
-
Abdel-Sater KA. The role of anti-aging approaches in managing hypogonadism in sedentary older males. Frontiers in Aging. 2024;5. doi:10.3389/fragi.2024.1514438
-
Santi D, Spaggiari G, Furini C, Griseta V, Zizzi E, Raffaele MGA, et al. Temporal trends in serum testosterone and luteinizing hormone levels indicate an ongoing resetting of hypothalamic-pituitary-gonadal function in healthy men: a systematic review. Endocrine Abstracts. 2025. doi:10.1530/endoabs.110.ep1326
-
Bhasin S, Brito JP, Cunningham GR, Hayes FJ, Hodis HN, Matsumoto AM, et al. Testosterone Therapy in Men With Hypogonadism: An Endocrine Society* Clinical Practice Guideline. The Journal of Clinical Endocrinology & Metabolism. 2018;103(5):1715-1744. doi:10.1210/jc.2018-00229
-
Mulhall JP, Trost LW, Brannigan RE, Kurtz EG, Redmon JB, Chiles KA, et al. Evaluation and Management of Testosterone Deficiency: AUA Guideline. Journal of Urology. 2018;200(2):423-432. doi:10.1016/j.juro.2018.03.115
-
Cappola AR, Auchus RJ, El-Hajj Fuleihan G, Handelsman DJ, Kalyani RR, McClung M, et al. Hormones and Aging: An Endocrine Society Scientific Statement. The Journal of Clinical Endocrinology & Metabolism. 2023;108(8):1835-1874. doi:10.1210/clinem/dgad225
-
Travison TG, Vesper HW, Orwoll E, Wu F, Kaufman JM, Wang Y, et al. Harmonized Reference Ranges for Circulating Testosterone Levels in Men of Four Cohort Studies in the United States and Europe. The Journal of Clinical Endocrinology & Metabolism. 2017;102(4):1161-1173. doi:10.1210/jc.2016-2935
-
Su L, Zhang S, Zhu J, Wu J, Jiao Y. Effect of partial and total sleep deprivation on serum testosterone in healthy males: a systematic review and meta-analysis. Sleep Medicine. 2021;88:267-273. doi:10.1016/j.sleep.2021.10.031
-
Hernández‐Pérez JG, Taha S, Torres‐Sánchez LE, Villasante‐Tezanos A, Milani SA, Baillargeon J, et al. Association of sleep duration and quality with serum testosterone concentrations among men and women: NHANES 2011–2016. Andrology. 2023;12(3):518-526. doi:10.1111/andr.13496
-
Potter NJ, Tomkinson GR, Dufner TJ, Walch TJ, Roemmich JN, Wilson PB, et al. Effects of Exercise Training on Resting Testosterone Concentrations in Insufficiently Active Men: A Systematic Review and Meta-Analysis. Journal of Strength & Conditioning Research. 2021;35(12):3521-3528. doi:10.1519/jsc.0000000000004146
-
Hayes LD, Elliott BT. Short-Term Exercise Training Inconsistently Influences Basal Testosterone in Older Men: A Systematic Review and Meta-Analysis. Frontiers in Physiology. 2019;9. doi:10.3389/fphys.2018.01878
-
Ikehata Y, Hachiya T, Kobayashi T, Ide H, Horie S. Body composition and testosterone in men: a Mendelian randomization study. Frontiers in Endocrinology. 2023;14. doi:10.3389/fendo.2023.1277393
-
Okobi OE, Khoury P, De la Vega RJ, Figueroa RS, Desai D, Mangiliman BDA, et al. Impact of Weight Loss on Testosterone Levels: A Review of BMI and Testosterone. Cureus. 2024. doi:10.7759/cureus.76139
-
Whittaker J. High-protein diets and testosterone. Nutrition and Health. 2022;29(2):185-191. doi:10.1177/02601060221132922
-
Whittaker J, Wu K. Low-fat diets and testosterone in men: Systematic review and meta-analysis of intervention studies. The Journal of Steroid Biochemistry and Molecular Biology. 2021;210:105878. doi:10.1016/j.jsbmb.2021.105878
-
Lincoff AM, Bhasin S, Flevaris P, Mitchell LM, Basaria S, Boden WE, et al. Cardiovascular Safety of Testosterone-Replacement Therapy. New England Journal of Medicine. 2023;389(2):107-117. doi:10.1056/nejmoa2215025
-
Pencina KM, Travison TG, Cunningham GR, Lincoff AM, Nissen SE, Khera M, et al. Effect of Testosterone Replacement Therapy on Sexual Function and Hypogonadal Symptoms in Men with Hypogonadism. The Journal of Clinical Endocrinology & Metabolism. 2023;109(2):569-580. doi:10.1210/clinem/dgad484
-
Cruickshank M, Hudson J, Hernández R, Aceves-Martins M, Quinton R, Gillies K, et al. The effects and safety of testosterone replacement therapy for men with hypogonadism: the TestES evidence synthesis and economic evaluation. Health Technology Assessment. 2024:1-210. doi:10.3310/jryt3981
-
Elagizi A, Köhler TS, Lavie CJ. Testosterone and Cardiovascular Health. Mayo Clinic Proceedings. 2018;93(1):83-100. doi:10.1016/j.mayocp.2017.11.006
-
Basheer B, Ila V, Barros R, Mesquita F, Lopes LS, Lima VFN, et al. Management of Adverse Effects in Testosterone Replacement Therapy. International braz j urol. 2025;51(3). doi:10.1590/s1677-5538.ibju.2025.9904
-
Desai A, Yassin M, Cayetano A, Tharakan T, Jayasena CN, Minhas S. Understanding and managing the suppression of spermatogenesis caused by testosterone replacement therapy (TRT) and anabolic–androgenic steroids (AAS). Therapeutic Advances in Urology. 2022;14. doi:10.1177/17562872221105017
-
Hashimi MA, Pinggera G, Shah R, Agarwal A. Clinician’s guide to the management of azoospermia induced by exogenous testosterone or anabolic–androgenic steroids. Asian Journal of Andrology. 2025;27(3):330-341. doi:10.4103/aja2024104
-
Fink J, Ide H, Horie S. Management of Male Fertility in Hypogonadal Patients on Testosterone Replacement Therapy. Medicina. 2024;60(2):275. doi:10.3390/medicina60020275
-
Coward R, McBride J. Recovery of spermatogenesis following testosterone replacement therapy or anabolic-androgenic steroid use. Asian Journal of Andrology. 2016;18(3):373. doi:10.4103/1008-682x.173938
-
Ledesma BR, Weber A, Venigalla G, Muthigi A, Thomas J, Narasimman M, et al. Fertility outcomes in men with prior history of anabolic steroid use. Fertility and Sterility. 2023;120(6):1203-1209. doi:10.1016/j.fertnstert.2023.09.016
-
Scarth M, Hauger LE, Thorsby PM, Leknes S, Hullstein IR, Westlye LT, et al. Supraphysiological testosterone levels from anabolic steroid use and reduced sensitivity to negative facial expressions in men. 2023. doi:10.31234/osf.io/h854w
-
Alves JV, da Costa RM, Pereira CA, Fedoce AG, Silva CAA, Carneiro FS, et al. Supraphysiological Levels of Testosterone Induce Vascular Dysfunction via Activation of the NLRP3 Inflammasome. Frontiers in Immunology. 2020;11. doi:10.3389/fimmu.2020.01647
-
National Board for Health & Wellness Coaching. NBHWC Health & Wellness Coach Scope of Practice. 2023. https://nbhwc.org/scope-of-practice/
-
Gulati M. Lifestyle Medicine’s Role in Common Hormonal Disorders: A Case-Based Discussion. American Journal of Lifestyle Medicine. 2024;18(5):638-647. doi:10.1177/15598276241242012